Disclaimer: This guide is for informational purposes only and does not constitute medical or legal advice. Consult with qualified professionals for guidance specific to your practice’s needs.
VMA training for healthcare professionals is a specialized program designed to equip remote administrative staff with the skills to manage clinical workflows, ensure HIPAA compliance, and integrate seamlessly with on-site medical teams to maximize practice efficiency. Is your practice drowning in a sea of administrative paperwork, patient calls, and scheduling conflicts? This relentless administrative burden not only pulls your focus from patient care but also leads to staff burnout, increases the risk of costly errors, and ultimately diminishes the quality of service you provide. The solution lies in a strategic integration of a professionally trained Virtual Medical Assistant (VMA), a move that can revolutionize your workflow, restore operational efficiency, and fortify your compliance standards.
What is a Virtual Medical Assistant and Why is This Role Critical in 2026?

A Virtual Medical Assistant is a highly skilled, remote professional who handles a wide array of non-clinical administrative tasks for a healthcare practice. Unlike an in-office medical assistant who may split time between the front desk and clinical support, a VMA is exclusively focused on streamlining the back-office and patient-facing digital operations that keep a modern practice running smoothly. This distinction is crucial for optimizing your team’s resources.
The role of the VMA has become mission-critical in today’s healthcare landscape. The rapid adoption of telehealth services and the increasing pressure to improve efficiency means that practices must find innovative ways to manage administrative functions without expanding their physical footprint. As explored in The Rise of Virtual Medical Assistants in Healthcare, VMAs offer a scalable, cost-effective solution that allows physicians and on-site staff to dedicate their valuable time to what matters most: direct patient care.
The Core Curriculum: Essential Components of an Effective VMA Training Program
A VMA is only as effective as their training. A comprehensive program goes far beyond basic administrative skills, instilling a deep understanding of the unique demands of a healthcare environment. The curriculum must be built on three core pillars to ensure a VMA is not just an assistant, but a secure and efficient extension of your clinical team.
Mastery of HIPAA-Compliant Workflows
This is the non-negotiable foundation of all VMA training. It involves rigorous education on the Health Insurance Portability and Accountability Act (HIPAA) and its practical application in daily tasks. Training covers protocols for handling Protected Health Information (PHI), using secure communication channels like encrypted messaging and VoIP phone systems, and maintaining strict privacy standards when accessing and updating Electronic Health Records (EHR).
Advanced Task Management for Clinical Settings
A proficient VMA is trained to manage the entire administrative lifecycle of a patient encounter. This includes advanced appointment scheduling across multiple provider calendars, pre-authorizing procedures, and performing detailed insurance eligibility verifications to prevent billing issues. They receive in-depth training on precise EHR data entry and management, as well as providing essential billing support by ensuring claims information is accurate and complete. These are some of the 10 Administrative & Clinical Tasks for Medical VAs that can be expertly handled remotely.
Professional Patient Communication Protocols
A VMA is often the first point of contact for a patient. Therefore, training must heavily emphasize soft skills tailored to healthcare. This includes developing a tone of empathy and professionalism for all phone and digital interactions, providing clear and concise information, and knowing precisely when and how to escalate a patient concern to the appropriate clinical staff member.
The Care VMA Advantage: A Proven Blueprint for Seamless Integration
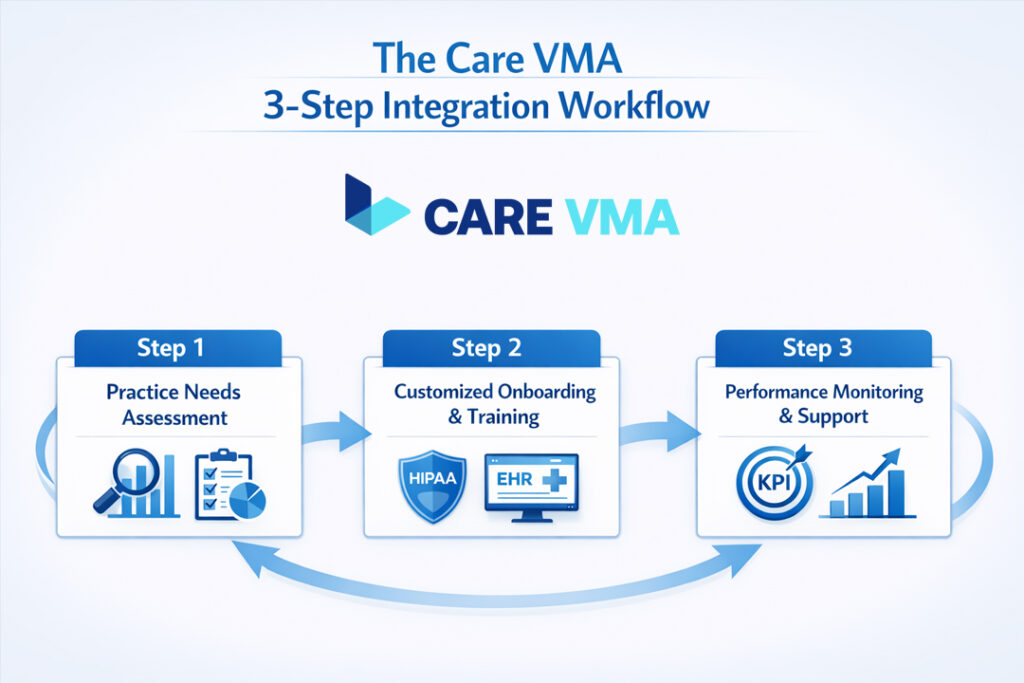
Simply hiring a VMA is not enough; success depends on a structured integration process. At Care VMA, we have developed a proven blueprint that ensures your new remote team member delivers measurable results from day one. We don’t just provide staff; we deliver a fully integrated workflow solution.
Step 1: In-Depth Practice Needs Assessment
Our process begins by analyzing your practice’s unique operational challenges and administrative bottlenecks. We map out your existing workflows, identify areas for improvement, and define the specific tasks where a VMA can provide the greatest impact. This ensures the VMA’s role is perfectly tailored to your needs.
Step 2: Our Rigorous, Role-Specific Onboarding & Training
Based on the needs assessment, we implement a role-specific training program. Our curriculum is designed to fill the gaps left by competitors, with a hyper-focus on your specific EHR system and internal communication protocols. This specialized training, grounded in the latest security practices, significantly reduces the learning curve and prepares the VMA to contribute effectively immediately, which is shown to boost overall clinic efficiency and reduce physician burnout.
Step 3: Performance Monitoring & Continuous Support
Our partnership extends well beyond onboarding. We establish key performance indicators (KPIs) to track success, such as reduced patient call wait times, improved data entry accuracy, and faster insurance verification turnaround. This data-driven approach allows us to continuously optimize the workflow and demonstrate a clear return on your investment, cementing our role as your long-term strategic partner.
FAQ: Answering Your Key Questions on VMA Training
What specific EHR software are VMAs trained on?
Our VMAs are trained on the industry’s leading EHR platforms, including Epic, Cerner, and eClinicalWorks. Furthermore, our agile training methodology includes a rapid adaptation process, allowing our assistants to quickly master any proprietary or specialized system your practice uses.
How is patient data kept secure when working with a remote VMA?
Security is our top priority. We ensure data protection through a multi-layered approach that includes the mandatory use of encrypted VPNs, adherence to HIPAA-compliant communication platforms, and strict data handling protocols that are a core component of our rigorous training and continuous monitoring.
Can a VMA handle clinical tasks like giving medical advice?
Absolutely not. Our training program draws a clear and immovable line between administrative and clinical duties. VMAs are strictly prohibited from performing any task that could be construed as practicing medicine, including offering medical advice, interpreting lab results, or diagnosing conditions. Their role is to manage administrative workflows to ensure patient safety and regulatory compliance.
Conclusion & Your Next Step to a More Efficient Practice
In 2026, integrating a professionally trained Virtual Medical Assistant is no longer a luxury-it is a strategic necessity for any healthcare practice aiming to thrive. It is the definitive step toward optimizing your resources, alleviating staff burnout, and refocusing your team on the ultimate mission: delivering exceptional patient care.
Stop letting administrative tasks control your practice. Schedule a free, no-obligation discovery call with our VMA integration specialists today and learn how we can customize a HIPAA-compliant workflow for you. Explore our Virtual Medical Assistant Services | Care VMA Health to take the first step.

![VMA Training for Healthcare Professionals [Official Guide]](https://carevmahealth.com/wp-content/uploads/2024/09/VMA-Training-for-Healthcare-Professionals-1024x683.jpg)
