For most healthcare providers, the majority of work for patients with chronic conditions happens between visits. The unbilled phone calls, the medication clarifications, the coordination with specialists—it’s a constant stream of administrative work that drains resources and leads to staff burnout. You know this proactive care is critical, but the uncompensated time makes it unsustainable.
Chronic Care Management (CCM) is the Centers for Medicare & Medicaid Services (CMS) program designed to solve this exact problem. From a provider’s perspective, CCM is a framework that reimburses your practice for the essential, non-face-to-face care you already provide to your most complex patients, turning an administrative burden into a structured, revenue-generating service line.
Beyond the Buzzword: What Does CCM Mean for Your Practice’s Bottom Line?
At its core, Chronic Care Management represents a fundamental shift from reactive, in-person appointments to proactive, continuous care—and finally getting paid for that work. It formalizes the time your clinical staff spends on care coordination, medication management, and patient education outside of a traditional office visit.
Imagine every 5-minute follow-up call, medication refill request, and email to a specialist being automatically tracked, documented, and contributed to your monthly revenue. That’s the power of a well-run CCM program. It’s not about adding more tasks; it’s about capturing the value of work you’re already doing to improve patient outcomes.
The Foundations: Is Your Practice & Patient Panel Eligible?
Before launching a CCM program, the first operational step is to confirm eligibility for both your patients and your practice. CMS has clear guidelines, but they are simple to navigate.
CMS Eligibility Checklist for Patients: The 3 Core Requirements
A patient must meet all three of these criteria to qualify for CCM services under Medicare:
- [ ] Diagnosis: The patient has two or more chronic conditions.
- [ ] Duration: These conditions are expected to last for at least 12 months or until the end of the patient’s life.
- [ ] Risk: The conditions place the patient at significant risk of death, acute exacerbation, or functional decline.
Common qualifying conditions include, but are not limited to:
- Hypertension
- Diabetes
- Heart Disease / Heart Failure
- Arthritis
- Asthma / COPD
- Dementia / Alzheimer’s
- Depression
- Chronic Kidney Disease
Provider Requirements: Who Can Bill for CCM Services?
CCM services can be billed by physicians, Physician Assistants (PAs), Nurse Practitioners (NPs), and other qualified healthcare professionals. Critically, the non-face-to-face services themselves can be performed by clinical staff under the “general supervision” of the billing provider.
This is where the operational model becomes flexible. “General supervision” does not require the supervising provider to be in the same building. This rule is what makes it possible to leverage highly trained, HIPAA-compliant external staff, such as a Virtual Medical Assistant, to execute the program without hiring additional full-time employees.
The Problem: The Hidden Costs of an In-House CCM Program
While the promise of new revenue is appealing, many practices that attempt a “do-it-yourself” CCM program quickly find themselves overwhelmed. This is where most in-house programs fail. The idea sounds simple, but the operational reality is a different story.
The “CCM Time-Sink”: Why Most In-House Programs Falter
The primary fear of any practice manager is adding another complex, time-consuming workflow to an already stretched team. Without a dedicated system, CCM can easily become that workflow.
Here are the operational challenges that cause in-house programs to become unprofitable:
- The Documentation Nightmare: Manually logging every minute of non-face-to-face time is tedious and prone to error. A 3-minute phone call, a 5-minute chart review, and a 2-minute email—each must be meticulously logged. Missed entries mean lost revenue and compliance risks.
- The Workflow Disruption: Pulling your on-site Medical Assistants away from rooming patients or assisting with in-office procedures to make CCM calls creates bottlenecks. This robs your practice of in-person efficiency to chase remote-care minutes.
- The Compliance Risk: Inaccurate or incomplete time-tracking is a major red flag during a CMS audit. Without an audit-proof system, your practice is at risk of failed audits, payment clawbacks, and significant financial penalties. This is one of the key ways how medical virtual assistants reduce burnout in US healthcare practices—by removing this high-stakes administrative burden.
The Solution: An Operational Blueprint for VMA-Powered CCM
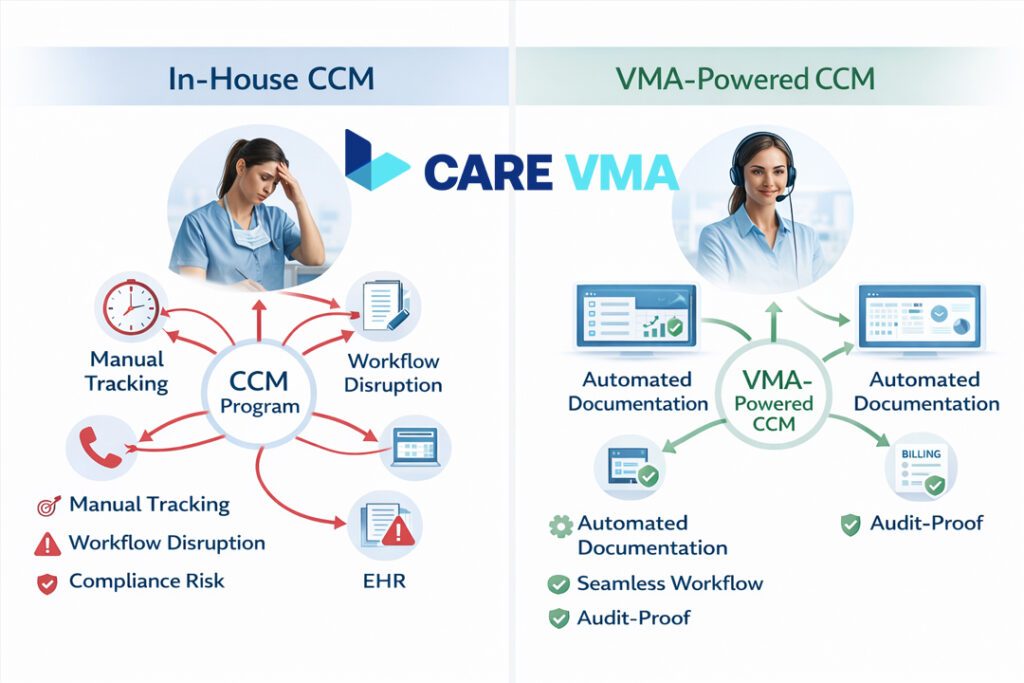
The key to a successful CCM program is not just understanding the rules but operationalizing them for maximum efficiency and profitability. Instead of viewing CCM as another task, think of it as a system—a system that can be expertly managed by a dedicated Virtual Medical Assistant (VMA).
How a Virtual Medical Assistant Transforms CCM from a Burden to a Benefit
A virtual chronic care management assistant is more than just software; it’s an integrated, remote team member who executes the entire CCM workflow on your behalf. They operate within your EHR and phone systems, acting as a true extension of your practice while freeing your in-house team to focus on the patients in front of them.
The Step-by-Step VMA Workflow (From Consent to Claim)
Here is the operational blueprint a dedicated VMA follows to run a compliant and profitable CCM program for your practice:
- Patient Identification & Enrollment: The VMA runs reports within your EHR to identify all eligible patients based on their diagnosis codes. They then handle the patient outreach, explain the program benefits, obtain verbal consent, and document it in the patient’s chart.
- Comprehensive Care Plan: Using data from the EHR, the VMA drafts the comprehensive care plan required by CMS. This plan is then sent to the billing provider for a quick review and signature.
- Monthly Patient Engagement: The VMA conducts the required 20+ minutes of monthly, non-face-to-face engagement. This includes check-in calls, medication adherence reminders, and coordinating with other providers.
- Automated Time-Tracking & Documentation: Every single interaction—every call, every email, every chart note—is automatically and contemporaneously logged in a HIPAA-compliant system. There is no manual time tracking.
- Billing Report Generation: At the end of the month, the VMA provides your biller with a clean, audit-proof report detailing every patient who met the time requirements for billing. No manual calculation or guesswork is needed.
The Financials: CCM Billing Codes & True ROI
Understanding the billing codes is straightforward. The real value comes from calculating the total return on investment, which goes far beyond direct reimbursement.
A Simple Guide to the Most Common CCM CPT Codes
While there are several codes, most practices will primarily use the following for non-complex CCM. Reimbursement rates vary by region, but this table provides a general estimate. For more detailed information, see our guide on navigating Chronic Care Management codes.
| CPT Code | Time Requirement (per calendar month) | Typical Medicare Reimbursement | Description |
|---|---|---|---|
| 99490 | At least 20 minutes of clinical staff time | ~$64 | The base code for non-complex CCM. |
| 99439 | Each additional 20 minutes of clinical staff time | ~$48 | Add-on code for patients requiring more time. |
Calculating Your Practice’s True ROI: Beyond Reimbursement
A profitable CCM program isn’t just about the revenue generated. It’s also about the significant costs you save. The true ROI comes from a more holistic calculation:
(CCM Revenue) + (Time Saved for In-house Staff x Their Hourly Rate) – (VMA Service Cost) = True ROI
When you factor in the value of freeing up your lead MA or nurse to assist with in-office procedures or patient care—work they were hired to do—the financial and operational benefits of outsourcing CCM administration become undeniable.
Don’t guess your potential. Use our 3-Minute CCM Revenue Calculator to see your practice’s specific numbers.
Integrating CCM into Your Practice with Care VMA Health
A successful CCM program is a powerful tool for improving patient health, reducing staff burnout, and strengthening your practice’s financial stability. But its success depends entirely on the operational workflow behind it.
Your Partner in Proactive Care & Practice Efficiency
Care VMA Health provides a turnkey solution that handles every administrative aspect of Chronic Care Management. We provide dedicated, HIPAA-trained Virtual Medical Assistants who integrate seamlessly with your EHR and existing workflows. There is no new software to learn and no new staff to hire or manage. We deliver a fully compliant, audit-proof program that allows you to focus on patient care while we generate a new, predictable revenue stream for your practice.
See It In Action: What Does a VMA-Powered Practice Look Like?
Dr. Smith’s practice used to spend 15 hours a week on unbilled patient follow-up. Their lead nurse was constantly interrupted to handle calls from their most complex patients.
After partnering with Care VMA Health, their dedicated VMA now manages their 200 CCM-enrolled patients. This generates over $12,000 per month in new, predictable revenue. More importantly, it has freed up their lead nurse to launch a new in-office wellness program, improving both patient satisfaction and practice growth.
Frequently Asked Questions
How much work is this for my staff?
With a VMA-powered program, the work for your in-house staff is minimal. The VMA handles patient identification, enrollment, monthly calls, and documentation. Your team’s involvement is primarily for clinical escalations and final review, just as you would with an in-house team member.
Is this HIPAA compliant?
Absolutely. All Care VMA Health assistants are fully trained in HIPAA regulations and operate on secure, encrypted platforms. We sign a Business Associate Agreement (BAA) with every practice to ensure total compliance and data security.
How does this integrate with my EHR?
Our VMAs are trained on all major EHR systems. They are granted secure, role-based access to your EHR, just like any other remote staff member, and document all activities directly within the patient’s chart to ensure a single source of truth.
What’s the difference between CCM and RPM?
Chronic Care Management (CCM) is a time-based service focused on the overall coordination of care. Remote Patient Monitoring (RPM) involves collecting and reviewing physiologic data (like blood pressure or glucose levels) from patients at home. While distinct, they are highly complementary. Combining CCM with the benefits of remote patient monitoring can provide a more comprehensive view of patient health and unlock additional revenue opportunities.
Your Next Steps
You’re already doing the work of chronic care. The only question is whether your practice is being compensated for it in a way that is efficient, compliant, and profitable.
Ready to Launch a CCM Program That Actually Works?
If you’re ready to turn an administrative burden into a powerful operational asset, we offer two clear next steps:
- Schedule a Free, No-Obligation Consultation. Let our experts build your practice’s custom CCM workflow and ROI projection in just 15 minutes.
- Explore our VMA services. See how a dedicated assistant can transform more than just your CCM program.


