A chaotic waiting room, phones ringing off the hook, and a burned-out administrative team—this is the daily reality for many clinics. The culprit isn’t a lack of effort; it’s a broken scheduling system. Your schedule is more than a calendar; it’s the operational engine driving patient flow, provider productivity, and practice revenue. Fighting with it costs you money, stresses your staff, and creates poor patient experiences. This guide provides a complete operational framework to move from chaos to control.Medical appointment scheduling is an operational system for managing patient flow, optimizing provider time, and maximizing revenue. A successful scheduling framework goes beyond a simple calendar; it combines proven models like Wave or Cluster scheduling with strategic no-show management, automated patient communication, and clear KPIs to reduce administrative burnout and improve the patient experience.
Why Your Scheduling Isn’t Just a Calendar—It’s Your Clinic’s Engine
Imagine a Tuesday morning. In Clinic A, the front desk staff is apologizing to a waiting room full of frustrated patients because the provider is running 45 minutes behind. Two appointments have already no-showed, leaving costly gaps in the schedule, and the phone is ringing with patients trying to reschedule. The administrative load is overwhelming, leading to mistakes and team burnout.
Now, consider Clinic B. A provider is running late due to an emergency, but every patient in the waiting room was notified by text 30 minutes before their arrival time. When a last-minute cancellation occurred, the slot was automatically filled within minutes by a patient on the waitlist. The front desk staff is calm, focused, and attending to the patients in front of them.
The difference isn’t luck; it’s the system. Inefficient scheduling is a primary source of administrative waste and a major contributor to the estimated $150 billion lost annually to no-shows in the U.S. healthcare system. This guide delivers the operational framework to build the smooth-running, profitable engine your clinic deserves.
Step 1: Choose the Right Scheduling Model (The Blueprint)
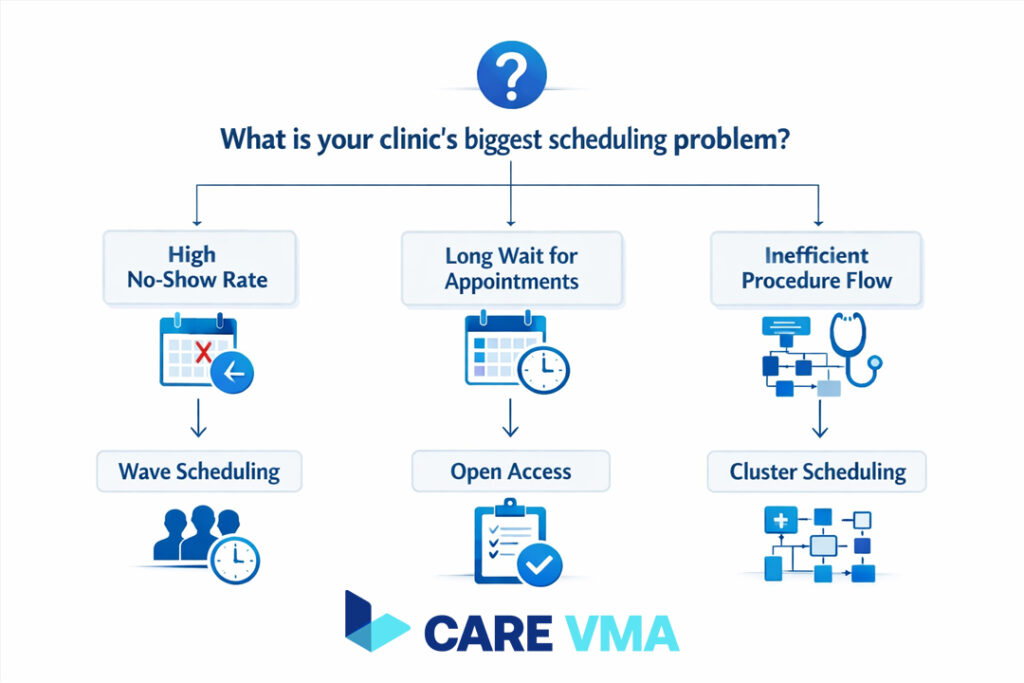
Stop forcing your clinic’s unique workflow into a rigid 15-minute box. The first step towards optimization is matching your scheduling model to the reality of your practice, whether you’re a high-volume primary care office or a procedure-heavy specialty clinic.
This is where most practices first go wrong—they adopt a one-size-fits-all approach that doesn’t account for their specific patient needs or provider rhythms.
| Scheduling Model | Best For | Operational Workflow |
|---|---|---|
| Stream (Time-Slot) | Specialty clinics with predictable visit lengths | One patient per time slot (e.g., 9:00, 9:15, 9:30). Simple and structured but inflexible. |
| Wave | High-volume primary care, labs | Schedule 3-4 patients at the top of the hour. They are seen in the order they arrive. Absorbs no-shows. |
| Modified Wave | Multi-provider practices | A hybrid model. Schedule two patients at the top of the hour and two at the half-hour. Balances access and flow. |
| Cluster (Block) | Practices with specific procedures | Group similar appointment types (e.g., all new patient physicals on Monday mornings). Maximizes staff and equipment efficiency. |
| Open Access (Hybrid) | High-demand clinics needing same-day access | A portion of the day is left open for same-day bookings, reducing wait times for urgent needs. |
How do you choose? It’s about identifying your primary point of friction.
- If your biggest problem is provider downtime from no-shows, use the Wave or Modified Wave model to create a buffer.
- If your providers complain about inefficient room turnover for procedures, implement Cluster scheduling.
- If patient complaints are about long waits for the next available appointment, integrate Open Access slots.
Step 2: Implement Staff-Facing Best Practices (The Daily Workflow)
These aren’t just ‘tips.’ This is the 10-minute daily routine that prevents 8 hours of chaos and empowers your front-desk team.
- The Noon-Backward/Forward Rule: Schedule morning appointments from noon backward and afternoon appointments from noon forward. This simple rule is a game-changer for protecting provider and staff time. It concentrates appointments in the middle of the day, leaving the start and end of the day open for administrative catch-up, team meetings, or squeezing in urgent cases without derailing the entire schedule.
- Strategic Buffer Slots: Don’t think of these as “catch-up time”; they are revenue protection. Intentionally block one or two 15-minute slots in the late morning and mid-afternoon. These slots should only be opened on the day of the appointment to accommodate emergencies or absorb delays, preventing provider burnout and keeping the day on track.
- The 5-Minute Daily Huddle: Your team lead should use this quick huddle each morning to review the day’s schedule. The script is simple: “Okay team, today we have 3 new patients who will require extra time. Mrs. Davis at 11:00 is a chronic late arrival, let’s be prepared. We have two open slots at 2:15 and 4:30—let’s check the recall list.” This aligns the entire team on potential risks and opportunities.
- Standardize Visit Lengths: Create appointment templates in your EHR/EMR system. For example, a “New Patient” visit is 45 minutes, a “Follow-Up” is 15 minutes, and a “Wellness Exam” is 30 minutes. This prevents staff from under-booking complex appointments, a common cause of schedule overruns. Efficient EHR/EMR management is critical for this to work.
This is where administrative load becomes lighter. A Virtual Medical Assistant can automatically prepare the daily huddle notes by scanning the schedule for new patients or flagging patients with a history of no-shows. They can identify potential conflicts and present a summarized risk report to the team lead before the huddle even starts.
Step 3: Systematize No-Show & Late Arrival Management (Revenue Recovery)
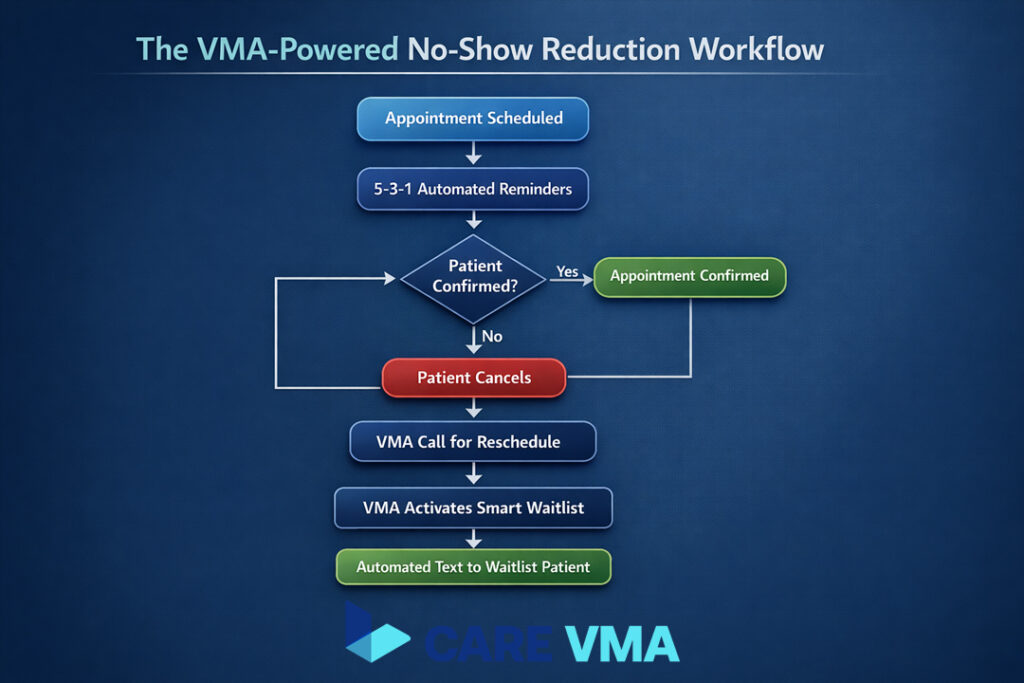
A 10% no-show rate can cost a single provider over $100,000 a year. That empty chair is a significant revenue leak. Here is the system to reclaim that lost income and maintain a full, productive schedule.
- The Automated 5-3-1 Reminder Strategy: The key to effective reminders is a multi-channel, escalating sequence.
- 5 Days Out: Send an automated email and/or text with appointment details.
- 3 Days Out: Send an automated text that requires a “YES” confirmation. This is critical—it turns a passive reminder into an active confirmation.
- 1 Day Out: Send a final reminder text with logistical details like “Please arrive 15 minutes early” or directions to the clinic.
- The VMA-Powered “Smart Waitlist”: This tactic addresses the critical content gap of managing provider downtime. When a patient cancels a confirmed appointment, a Virtual Medical Receptionist immediately initiates an automated workflow. The system identifies the next patient on the waitlist and sends a text: “An opening with Dr. Smith has become available today at 2:30 PM. Would you like to claim this spot? Reply YES to confirm.” This fills empty slots in minutes, not hours, turning lost revenue into productive time.
- The “Tetris” Method for Late Arrivals: Empower your front-desk staff. If the 10:00 AM patient is 10 minutes late and the 10:15 AM patient has already checked in, see the 10:15 patient first. This dynamic reordering keeps the provider working and prevents one late patient from creating a domino effect of delays.
- Chronic No-Show Policy: For patients who no-show more than twice, a clear policy is essential. A professional script might be: “Mr. Johnson, we’ve noted several missed appointments. To ensure all our patients have access to care, our policy for future appointments will be to place you on our same-day call list.” This is firm but focused on providing care.
Step 4: Master Patient Communication (Managing the Experience)
Here’s an insight often missed: patient satisfaction isn’t about zero wait time; it’s about managing the psychology of the wait. Informed patients are patient patients. Frustration builds in silence.
- The 15-Minute Rule: As soon as a provider is running more than 15 minutes behind, communication must begin. Don’t wait for the waiting room to fill up with annoyed glances. Proactive communication is a sign of respect for your patients’ time.
- The “Waiting Room Concierge” Role: Empower a staff member to be the point of contact in the waiting area. Even better, leverage technology. A VMA can send out a broadcast text message, a key component of effective patient communication and customer service.
A real-world scenario shows the power of this system:
Scenario: Dr. Smith is running 30 minutes late due to an unexpected in-office procedure.
VMA Action: The front desk flags the delay in the system. The VMA automatically sends a batch text to all patients scheduled in the next 90 minutes: “Hi [Patient Name], an update from [Clinic Name]. Dr. Smith had an unexpected patient emergency, and we are running approx. 30 mins behind schedule. We apologize for the delay and appreciate your understanding.”
Result: Patients arrive informed, not frustrated. Some may choose to arrive later. The waiting room remains calm, and the front desk staff is freed from repeatedly delivering bad news.
Step 5: Track the 4 KPIs That Actually Matter
If you can’t measure your scheduling system, you can’t fix it. Many clinics track dozens of metrics, but focusing on these four essential Key Performance Indicators (KPIs) will give you 90% of the insights you need.
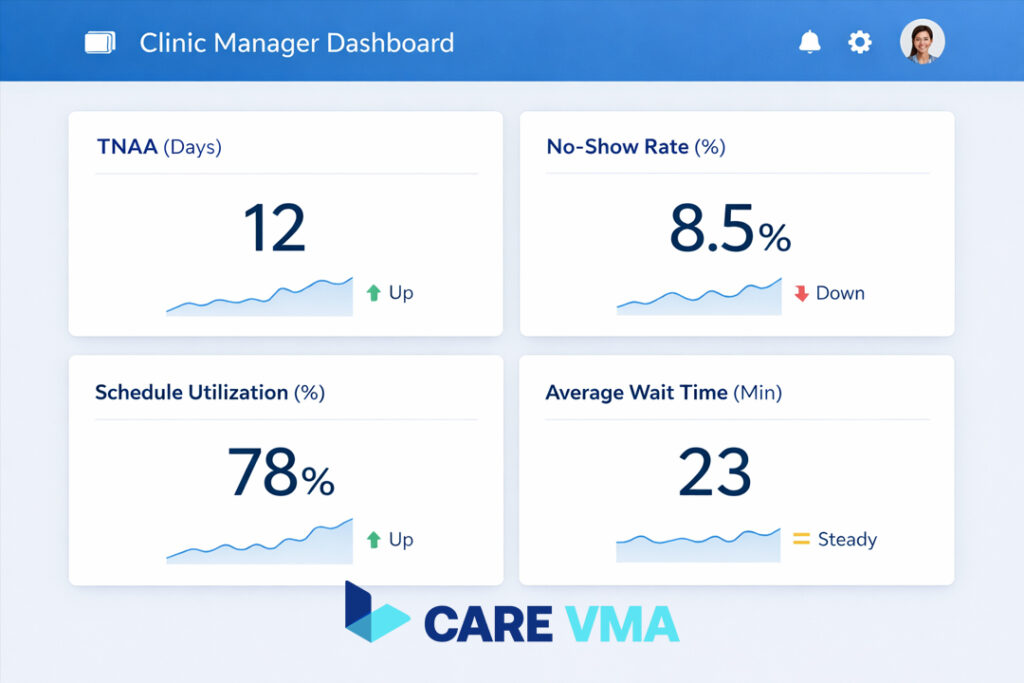
- TNAA (Third Next Available Appointment): This is the gold standard for measuring patient access. It measures the number of days a patient must wait to get the third available routine appointment. A high TNAA (e.g., >10 days) is a sign that your patient demand is outstripping your capacity.
- No-Show Rate: The ultimate measure of your revenue leakage. Calculate it as
(Total No-Shows / Total Scheduled Appointments) x 100. The industry benchmark is to keep this below 5%. - Schedule Utilization: This is your provider productivity metric. It measures the percentage of available appointment time that is actually filled with patients. A low rate may indicate problems with your patient recall or confirmation process. Aim for >90%.
- Average Wait Time: The #1 benchmark for patient experience. Track the time from a patient’s scheduled appointment to the moment they are seen by the provider. According to the AAFP, a wait time over 20 minutes is where satisfaction scores begin to plummet.
The Feedback Loop (This is the Game-Changer) This is where competitors’ advice falls short. Data is useless without action. Use this “if-then” framework:
- If your TNAA is over 10 days, it’s time to implement Open Access slots or analyze your appointment templates for inefficiencies.
- If your No-Show Rate is above 7%, your reminder system is broken. Implement the 5-3-1 reminder strategy immediately.
- If your Schedule Utilization is under 85%, your recall and waitlist systems are not working. It’s time to automate this with a service that can handle referral management and recalls.
- If your Average Wait Time is over 20 minutes, your team needs to enforce the 15-minute communication rule and use strategic buffer slots.
Putting It All Together: The VMA-Powered Scheduling Flywheel
This guide has laid out the models, workflows, and metrics for a high-performance scheduling system. Now, let’s tie it all together. The hub of this entire operational system is a Virtual Medical Assistant. A VMA from Care VMA doesn’t just perform tasks; they manage the system.
This creates a powerful “flywheel” effect:
- A VMA handles the high-volume, repetitive tasks: automated reminders, confirmations, smart waitlist management, proactive delay texts, and digital intake form distribution.
- This dramatically reduces the administrative load on your in-house staff, cutting down on burnout.
- Your freed-up staff can now focus on high-value, human-centric tasks: greeting patients warmly, managing complex check-ins, and delivering an exceptional in-person experience.
- This improved patient experience and hyper-efficient communication reduces no-shows and patient frustration.
- A more predictable, optimized schedule increases provider productivity and clinic revenue, which fuels further investment in a better patient experience.
Ready to implement an operational framework that actually works? A Virtual Medical Assistant from Care VMA can have this system running for your clinic in under a week, integrating with your existing EHR and workflows.
Schedule a free, no-obligation consultation to see a live demo of the VMA-Powered Scheduling Flywheel in action.
Appendix: Essential Front Desk Scripts & Checklists
Script: Handling an Urgent “Work-In” Request
“I’m sorry to hear you’re feeling unwell. Let me get some details to see how we can best help. (Assess for emergency symptoms). Dr. Smith’s schedule is fully committed today, but I can ‘work you in’ at 2:00 PM. This means you will be seen between our scheduled patients, so there may be a longer wait than usual. The provider will absolutely see you. Does that work for you?”
Script: New Patient Greeting and Booking Confirmation
“Thank you for choosing [Clinic Name]! I have you scheduled for your new patient visit with Dr. Jones on Tuesday the 12th at 10:00 AM. Please plan to arrive 15 minutes early at 9:45 AM to complete your registration. To save time, we will text you a link to our digital intake forms, which you can fill out at home. We look forward to seeing you.”
Checklist: Daily Schedule Huddle Agenda (5 Mins)
- [ ] Review number of new vs. established patients.
- [ ] Identify any “cluster” blocks (e.g., procedures) and confirm readiness.
- [ ] Flag any patients with a history of no-shows or late arrivals.
- [ ] Confirm buffer slots are still open.
- [ ] Review the waitlist and recall list for any opportunities to fill open slots.


