For a busy neurology practice, the referral process is both the primary source of growth and a significant operational bottleneck. Each fax, portal notification, or EHR alert represents a patient in need of specialized care, but managing this influx is a high-stakes challenge. Inefficient neurology referral tracking doesn’t just create administrative chaos; it leads to significant revenue loss, increased clinical risk for patients with urgent conditions, and frustrated referring physicians. The solution lies not in more complex software, but in a smarter, human-powered workflow driven by a Virtual Medical Assistant (VMA).
The High Cost of Inefficient Neurology Referral Tracking
![]()
When the intake process breaks down, the consequences ripple through the entire practice, affecting financial stability, patient outcomes, and staff morale. The manual methods that once worked are no longer sufficient to handle the volume and complexity of modern neurology.
Referral Leakage: Quantifying Lost Revenue from Unscheduled Patients
Referral leakage is the silent profit killer for specialty practices. When a referral is misplaced, follow-up is delayed, or a patient gets lost in a phone tag loop, they often seek care elsewhere or give up entirely. For a neurology practice, where a single new patient consultation and subsequent procedures can be worth thousands, even a small leakage rate translates into tens of thousands in lost revenue annually. Tracking these referrals from receipt to a scheduled appointment is critical to ending the manual, complex processes of referral management and capturing all potential revenue.
The Clinical Risk of Delayed Triage for Urgent Neurological Cases
The stakes in neurology are exceptionally high. A patient with symptoms of a transient ischemic attack (TIA) or a new-onset seizure cannot afford to wait in a queue behind a routine migraine follow-up. A manual, paper-based system makes it dangerously easy for urgent cases to be overlooked. Delayed triage can lead to postponed diagnosis and treatment, directly impacting patient outcomes. An efficient system must be able to immediately identify and flag high-acuity cases for expedited scheduling.
Administrative Burnout: Why Your Staff Can’t Keep Up with Manual Intake
Your front-office staff are likely overwhelmed. They are tasked with juggling incoming faxes, monitoring multiple patient portals, answering calls, and manually entering data into the EHR. This constant context-switching is inefficient and a primary driver of burnout. When staff are stretched thin, mistakes happen—referrals are missed, prior authorizations are delayed, and communication with referring PCPs falters. This administrative overload is a key reason many practices seek solutions that can reduce administrative burnout and restore operational sanity.
Beyond Spreadsheets: Why Neurology Referrals Are Uniquely Complex
Neurology isn’t like other specialties. The information required for a successful consultation is far more intricate than a simple referral note, making generic tracking systems and spreadsheets inadequate.
Managing Sub-Specialty Routing: From Epileptologists to Movement Disorder Specialists
A referral for “seizures” must be routed to an epileptologist, while a patient with Parkinson’s-like symptoms needs to see a movement disorder specialist. A manual system relies on the front desk staff’s clinical knowledge to make these critical routing decisions. A sophisticated tracking process automates this, ensuring patients are scheduled with the right expert from the very beginning, preventing unnecessary appointments and delays in care.
The Missing Data Dilemma: Chasing Down MRIs and EEG Reports
A neurology referral is often incomplete without corresponding diagnostic data. How often do patients arrive for their appointment, only for the neurologist to discover their MRI or EEG reports were never sent over? This results in a wasted appointment slot and a rescheduled visit. A proactive referral workflow involves chasing down this missing information before the appointment is even scheduled, ensuring the neurologist has a complete picture for a productive first visit.
The Challenge of Integrating Faxes, Portals, and EHR Notifications
Referrals arrive through a fragmented web of channels. A primary care physician might send a referral via fax, while a hospitalist uses an online portal, and another specialist sends a message directly through the EHR. Without a centralized system, staff must constantly monitor every channel, creating a high risk that a request will be missed. The key is to consolidate all incoming referrals into a single, manageable queue.
What is VMA-Powered Neurology Referral Tracking?
Neurology referral tracking powered by a Virtual Medical Assistant (VMA) is a specialized service where a remote, professionally trained assistant manages the entire patient referral lifecycle. This process includes capturing referrals from all sources, performing initial triage based on urgency, verifying that all necessary diagnostic data (like MRIs) is attached, scheduling the patient with the correct sub-specialist, and ensuring communication is closed with the referring physician. By entrusting this complex workflow to a dedicated resource, practices can modernize their neurology practice operations without hiring additional in-house staff.
The VMA Workflow: A Step-by-Step Guide to Perfecting Neurology Patient Intake
A Care VMA, acting as a dedicated Virtual Patient Care Coordinator, transforms your referral process from a reactive scramble into a proactive, standardized system. This workflow ensures no patient is left behind.
- Step 1: Centralized Digital Capture from All Referral Channels Your VMA establishes a single digital inbox. All faxes, portal messages, and emails are funneled into one queue, eliminating the need for staff to monitor multiple systems and preventing referrals from being lost.
- Step 2: Automated Triage & Urgency Flagging (Stroke vs. Stable Migraine) Working from your practice’s protocols, the VMA reviews each referral, immediately flagging urgent cases (e.g., suspected stroke, TIA, new-onset seizure) for priority review by clinical staff. Routine cases (e.g., stable migraine, chronic neuropathy) are queued for standard scheduling.
- Step 3: Proactive Data Verification (Requesting Missing Imaging Pre-Review) The VMA acts as a gatekeeper. If a referral mentions a recent MRI but the report isn’t attached, the VMA proactively contacts the referring provider’s office to obtain the missing files before the patient is scheduled.
- Step 4: Intelligent Scheduling with the Correct Sub-Specialist Based on the referral information and your protocols, the VMA schedules the patient with the appropriate neurologist (e.g., cognitive, epilepsy, headache specialist), ensuring an efficient use of your providers’ time and expertise. This is fundamental to optimizing the patient intake and scheduling process.
- Step 5: Closing the Loop: Automated Consult Note Delivery to the PCP The job isn’t done until the referring physician is informed. After the patient’s visit, the VMA ensures the consult note is transmitted back to the PCP, confirming the patient was seen and closing the referral loop. This simple step is crucial for building and maintaining strong referral relationships.
Use Case: Transforming a High-Volume Stroke Center’s Referral Process
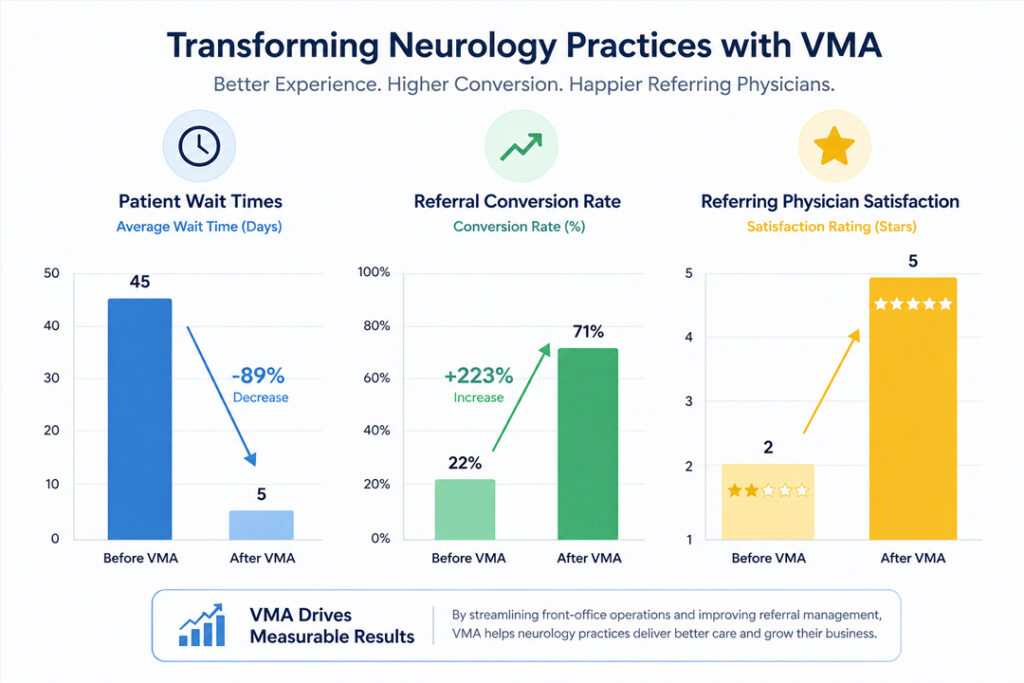
A busy, multi-physician stroke center was drowning in administrative chaos, threatening both its reputation and patient care standards.
- Before Care VMA: The center faced a constant backlog of over 200 unprocessed faxes. This led to significant delays in scheduling for TIA patients, who require urgent evaluation. Furthermore, there was no reliable system to track whether referring PCPs ever received the final consult notes, causing frustration among their primary referral sources.
- After Care VMA: By implementing a dedicated Virtual Medical Assistant, the practice achieved a “zero-inbox” for faxes daily. All urgent referrals were processed and scheduled within a 24-hour turnaround. They instituted a 99% close-the-loop rate for consult notes, leading to a noticeable increase in referral volume from satisfied and well-informed PCPs.
The Tangible Business Benefits for Your Neurology Practice
Implementing a VMA-powered system goes beyond simple organization; it delivers measurable improvements to your practice’s bottom line and clinical mission.
Reduce Patient Wait Times and Appointment Backlogs Through Efficient Triage
By systematically triaging and preparing every referral before it reaches the scheduling stage, a VMA ensures that appointment slots are used effectively. Patients with urgent needs are seen faster, while complete data for all patients reduces the chance of wasted, non-billable appointments, helping to clear backlogs and improve access to care.
Calculate the ROI: How a VMA Cuts Administrative Costs and Boosts Appointment Conversion Rates
A VMA is a fraction of the cost of a full-time in-house employee. By taking over the time-consuming administrative tasks of referral management, a VMA frees up your on-site staff to focus on high-value, patient-facing activities. This operational efficiency, combined with the capture of previously “leaked” referral revenue, delivers a powerful and rapid return on investment.
Increase Referring Physician Satisfaction with Flawless, Closed-Loop Communication
Referring providers want partners who are easy to work with. When they know their referral will be handled promptly, their patient will be scheduled correctly, and they will receive a consult note without having to ask, their confidence soars. A VMA-managed system makes your practice the preferred choice for neurology referrals, creating a sustainable engine for growth.
Ensuring HIPAA Compliance and Professionalism in VMA-Managed Workflows
Trust is paramount in healthcare. Care VMA operates on a foundation of security and professionalism. All our Virtual Medical Assistants are rigorously trained and operate under strict protocols for patient data handling. We are fully committed to ensuring HIPAA compliance and data security, utilizing secure communication channels and access-controlled systems to protect your patients’ sensitive information at every step of the referral process.
Ready to Build a More Efficient and Profitable Neurology Practice?
Stop letting referral leakage and administrative overload dictate the success of your practice. A dedicated Virtual Medical Assistant from Care VMA can streamline your neurology referral tracking, reduce patient wait times, and strengthen your relationships with referring physicians.
Frequently Asked Questions (FAQ)
How does a Care VMA integrate with our practice’s existing EHR like Epic or Cerner?
Our VMAs are trained on all major EHR platforms. They access your system securely and remotely, just like an in-house employee, to manage referral data, schedule appointments, and upload necessary documentation directly into the patient’s chart.
Can a Virtual Medical Assistant handle the clinical triage of complex neurology cases?
A VMA performs administrative and protocol-based triage. They are trained to identify keywords and urgency indicators (e.g., “TIA,” “new-onset seizure”) based on your specific clinical guidelines and immediately escalate those charts to your on-site clinical staff (like a nurse or neurologist) for final review and disposition.
What is the typical onboarding process for implementing a VMA for referral tracking?
Our onboarding is designed to be seamless. We start with a discovery call to understand your exact workflow, protocols, and sub-specialty needs. We then document these processes, train your dedicated VMA, and gradually integrate them into your live environment, ensuring a smooth transition with minimal disruption.
How does this model solve the problem of inappropriate referrals (e.g., general dizziness) being sent to our neurologists?
During the intake and data verification step, your VMA can screen referrals against your pre-defined acceptance criteria. If a referral for a condition you don’t treat (like general dizziness better suited for an ENT) comes in, the VMA can flag it and, per your protocol, communicate back to the referring office with guidance on the more appropriate specialty, saving valuable appointment slots.

