Paperwork should never be the bottleneck between a patient and the care they need. Yet, for countless medical practices, prior authorization submissions are consuming over 12 hours a week, leading to exhausted staff and dangerous delays in patient treatment. With the new 2026 CMS rules, emerging state-level “Gold Card” laws, and insurer-specific changes, this administrative maze has become more complex than ever. A single error can trigger a denial, a lengthy appeal, and more time stolen from your patients. But what if you could offload the entire process—from initial submission to the final appeal—to a team of dedicated experts who live and breathe these regulations?
Prior authorization is a cost-control process that health insurance companies use to verify the medical necessity of a service, procedure, or prescription before it is provided. For healthcare providers, however, it has evolved into a significant administrative burden that often stands in the way of timely patient care. This guide, fully updated for the 2026 regulatory landscape, synthesizes the latest information from the Centers for Medicare & Medicaid Services (CMS) and the American Medical Association (AMA) to provide a clear, actionable path forward.
How the Prior Authorization Process Actually Works (And Where It Breaks Down)
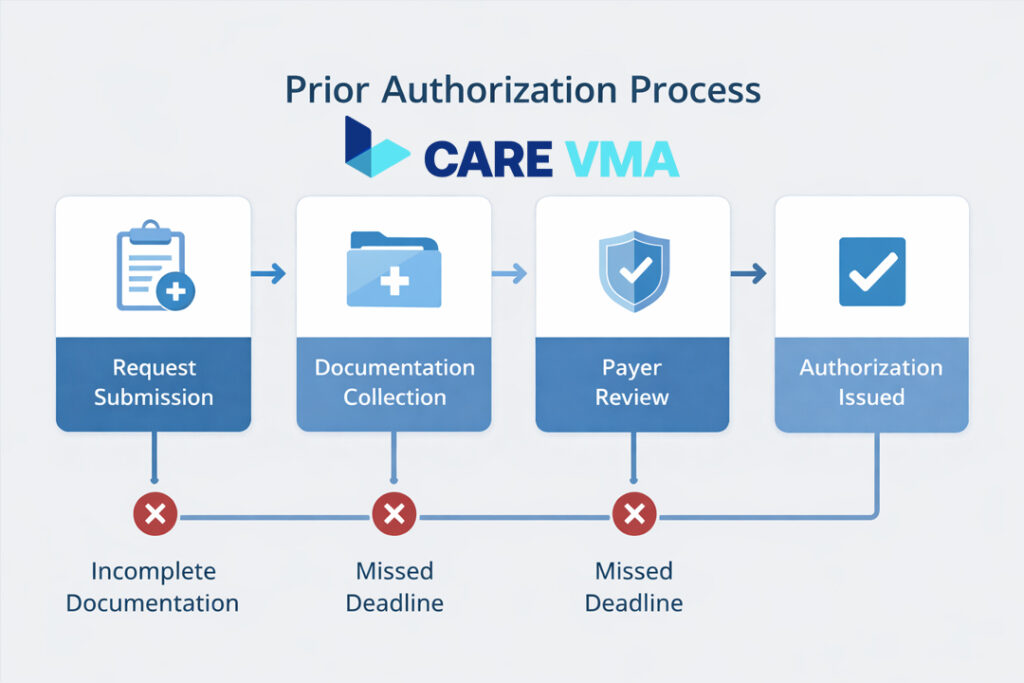
At first glance, the prior authorization workflow seems straightforward. But in reality, the process is riddled with potential failure points where simple mistakes can cause significant delays. Think of it as a series of gates, each one needing the right key at the right time.
The process, often referred to as pre-certification or prior approval, generally follows four steps:
- Order & Verification: A physician determines a patient needs a service requiring pre-approval, like an MRI or a specialty drug. The administrative team must first confirm that the patient’s health insurance plan requires PA for that specific service.
- Submission: The provider’s office compiles and submits the required clinical documentation to the insurer to prove medical necessity. This has historically been a manual process involving faxes, phone calls, and clunky payer portals.
- Insurer Review: The insurance company reviews the submission against its policies. This is where requirements like step therapy (forcing a patient to try a less expensive alternative first) are enforced.
- Decision & Action: The insurer issues a decision: approved, denied, or a request for more information. A denial often initiates a time-consuming appeal process, which can escalate to a peer-to-peer review between the treating physician and a medical director from the insurance company.
The most common breaking points are incomplete clinical documentation, missed deadlines, and submitting to the wrong department—small administrative errors that lead to an immediate denial of care and a reset of the entire clock.
The Real Cost: How PA Burdens Your Practice and Delays Patient Care
The hours spent on prior authorizations are just the beginning of the story. What most people don’t realize is that the true cost is measured in delayed patient care, worsening physician burnout, and declining staff morale.
It’s not just 12 hours of paperwork; it’s 12 hours your staff isn’t spending with patients at the front desk. It’s the profound frustration of telling a patient that their essential MRI is delayed—again. It is the burnout your most dedicated team members feel from fighting with insurers over treatments that are clearly a medical necessity.
The data paints a stark picture of this nationwide problem. According to a recent AMA survey:
- 94% of physicians report that the PA process causes delays in necessary care.
- 78% report that patients have abandoned their recommended course of treatment due to struggles with the pre-certification process.
- An average medical practice completes 43 prior authorizations per physician, per week, consuming over 12 hours of physician and staff time.
This isn’t just an inefficiency; it’s a barrier to quality healthcare that directly impacts patient outcomes and the financial health of your practice.
The 2026 Tectonic Shift: New CMS Rules, Gold Cards, and AI You Must Know
What worked for managing prior authorization yesterday is already becoming obsolete. A perfect storm of new federal mandates, progressive state laws, and disruptive technology is fundamentally changing the rules of the game for 2026 and beyond. Staying ahead of this curve is no longer optional.
New Federal Mandates: The CMS 72-Hour Rule
The most significant change comes from the CMS Interoperability and Prior Authorization Final Rule. Starting in 2026, it imposes strict deadlines on Medicare Advantage, Medicaid, and other government-sponsored plans. Payers must:
- Provide a PA decision within 72 hours for all urgent requests.
- Provide a decision within 7 calendar days for all standard (non-urgent) requests.
- Provide a specific, clinical reason for any denial.
This is a monumental shift away from the weeks-long black holes many practices currently face.
State-Level Relief: The Rise of “Gold Card” Laws
In parallel, states are taking matters into their own hands with “Gold Card” laws. These programs exempt physicians with consistently high approval rates (typically 90% or more) from PA requirements for specific services. States like Texas and Arkansas pioneered this approach, and many others are now following suit. Gold Carding rewards providers for accurate submissions and directly helps to reduce the administrative burden on high-performing practices.
Automation & AI: The Double-Edged Sword
Artificial intelligence is the wild card. On one hand, insurers like UnitedHealthcare and Cigna are using AI for PA automation, leading to near-instant approvals for routine requests. On the other hand, a backlash against using AI to issue auto-denials has led states like California and Maryland to pass laws requiring a human clinical reviewer to be involved in any denial decision.
Overwhelmed by these changes? Keeping track of federal rules, state laws, and individual payer policies is a full-time job. Discover how a dedicated virtual specialist can manage this complexity for you.
The Modern Solution: Offloading PA to Virtual Specialists
Keeping up with this evolving landscape isn’t a side-task—it’s a specialized, full-time job. That’s why forward-thinking practices are moving away from stretching their in-house team thin and are instead embracing a smarter, integrated approach with virtual prior authorization specialists.
This isn’t about “outsourcing” a task; it’s about embedding a strategic partner into your workflow. At Care VMA, our virtual specialists proactively manage the entire PA lifecycle to eliminate this burden from your staff.
Here’s how it works in practice:
- Manages Flawless Submissions: Our specialists gather and submit the complete and accurate clinical documentation required by each specific payer, drastically reducing the risk of an initial denial due to administrative error.
- Navigates the New Rules: The team is continuously trained on the 2026 CMS final rule, Gold Card laws for every applicable state, and the unique policies of major payers like Cigna and UnitedHealthcare.
- Handles Every Appeal: In the event of an improper denial, our specialists manage the entire appeal process from start to finish, including coordinating peer-to-peer reviews, freeing your physicians from hours on the phone.
Consider a multi-specialty clinic struggling with PAs for high-cost imaging and specialty drugs. After partnering with Care VMA, their approval time dropped by 50%, and their staff reclaimed over 40 hours per month. That time is now spent on high-value tasks like patient scheduling and communication, directly improving both revenue and patient satisfaction.
The Outcome: Reclaim Your Time, Reduce Burnout, and Accelerate Care
Offloading the process is one thing, but what tangible results can your practice expect? It boils down to three key areas where you’ll see a dramatic return on investment.
- Workflow Improvement: This is the most immediate benefit. Instead of your skilled staff spending half their day on hold with insurance companies, they are refocused on the patient-facing work they were hired to do. This not only boosts efficiency but also dramatically improves staff morale and reduces the burnout that leads to costly turnover.
- Cost Savings & Revenue Acceleration: By minimizing denials and successfully managing appeals, you ensure a faster, more predictable revenue cycle. You reduce the overhead costs associated with the hours your team spends on uncompensated administrative work. A streamlined PA process means you get paid correctly, and on time, for the care you deliver.
- Superior Patient Care: Here’s the thing that matters most. When prior authorizations are approved quickly, patients get the care they need, when they need it. This leads to better clinical outcomes, higher patient satisfaction scores, and a stronger reputation for your practice in the community.
In-House vs Managed PA: A Clear Comparison
The choice between managing prior authorizations internally or partnering with a specialist team becomes crystal clear when you look at a direct comparison of the resources and results.
| Feature | Managing In-House | With Care VMA Virtual Specialists |
|---|---|---|
| Staff Time | 12-15 hours/week | <1 hour/week (for handoff) |
| Expertise | General admin knowledge | Dedicated PA experts, rules updated daily |
| Denial Rate | Industry average (10-15%) | Significantly lower due to expert submissions |
| Staff Morale | High stress & burnout | High satisfaction, focus on patient-facing tasks |
Explore Further Resources
Ready to dive deeper? These resources provide the next level of detail on mastering modern healthcare administration and reducing operational friction in your practice.
- Service Page: Ready to see how our specialists handle insurance verification and prior authorization? Learn About Our Virtual Specialist Services.
- Related Article: Curious about other ways to improve your practice’s workflow? Discover How to Optimize Your Clinic’s Workflow and Cut Errors.
- Related Article: Facing too many claim denials? Learn About Denial Management and Prevention Strategies.
Frequently Asked Questions
What are the new prior authorization deadlines from CMS in 2026?
Starting in 2026, the CMS Final Rule mandates that Medicare Advantage and Medicaid plans must issue prior authorization decisions within 72 hours for urgent requests and 7 calendar days for standard (non-urgent) requests.
How does a “Gold Card” law work for physicians?
“Gold Card” laws exempt physicians who have a very high prior authorization approval rate (typically 80-90% for a specific service) from needing to submit PAs for that same service in the future, usually for a period of one year. It’s a system designed to reward high-performing providers and reduce their administrative workload.
Can an insurance company use AI to deny my prior authorization request?
While insurance companies are using AI to speed up approvals, several states have passed laws that prohibit the use of AI alone to deny care. For any denial based on medical necessity, a human clinical reviewer must verify the decision.
Conclusion
Prior authorization is no longer just another administrative task; it’s a complex, strategic challenge that directly impacts your practice’s financial health, staff well-being, and ability to deliver timely patient care. The regulatory and technological landscape is shifting faster than ever, but navigating it doesn’t have to drain your team’s energy and resources.
Stop letting paperwork dictate your practice’s efficiency and your patients’ care journeys. It’s time to reclaim your team’s time and refocus on the mission that brought you into medicine in the first place: caring for your patients.
Ready to eliminate the prior authorization bottleneck for good? Schedule a free, no-obligation consultation with our team to discover how our virtual specialists can take over your entire PA workflow, starting this week.


