Disclaimer: The information provided in this article is for informational purposes in the field of healthcare management and does not constitute individual financial advice.
High denial rates and ballooning days in accounts receivable are not just numbers on a report; they are the primary drags on your organization’s financial health. As a healthcare financial leader, you feel the constant pressure of tight margins, complex payer rules, and the operational strain on your team. You know there has to be a more efficient way forward. Revenue Cycle Management (RCM) Mastery is the strategic orchestration of clinical, administrative, and financial functions, which in 2026 is driven by AI automation and data analytics to achieve peak financial efficiency and operational resilience. This guide is your blueprint.
The Three Fundamental Pillars of RCM Mastery
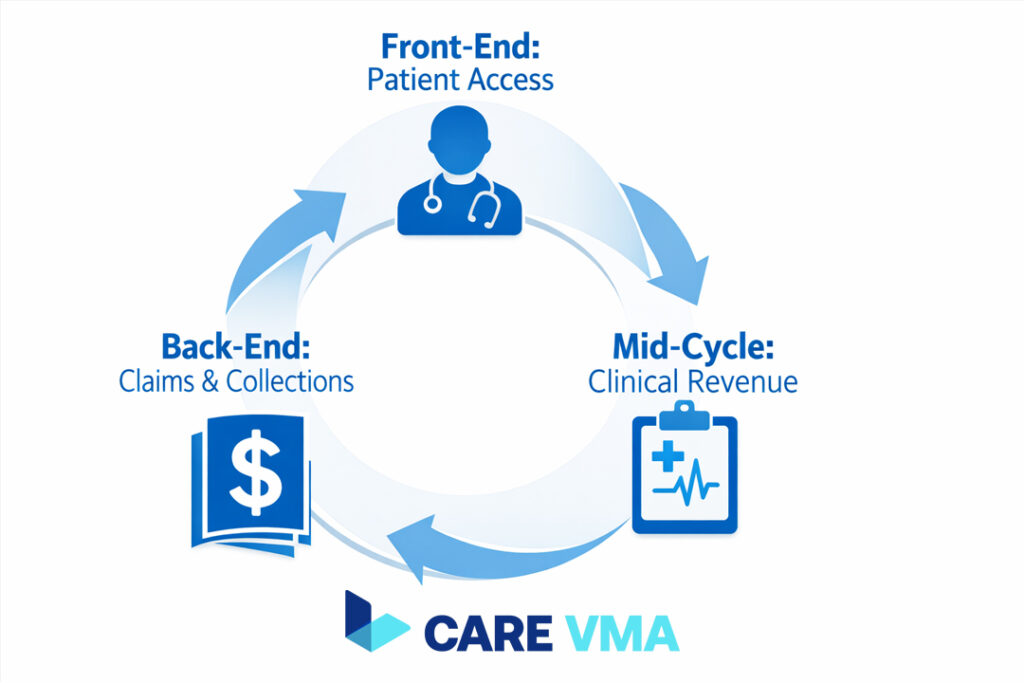
A resilient revenue cycle is built on a flawless foundation. Mastery requires optimizing every touchpoint, which is traditionally broken down into three critical phases. Understanding and reinforcing each pillar is non-negotiable for financial success.
Front-End (Patient Access): The Foundation of Clean Claims
This is where the cycle begins and, unfortunately, where most errors occur. Research from the Healthcare Financial Management Association (HFMA) indicates that up to 60% of claim denials originate from front-end inaccuracies. Mastery here involves perfecting patient registration, ensuring precise demographic data capture, and performing real-time insurance eligibility and benefits verification. Automating insurance verification and prior authorization is the first step to ensuring a claim is clean before a service is even rendered.
Mid-Cycle (Clinical Revenue): Accuracy from Service to Code
This phase bridges clinical care with financial documentation. It includes charge capture, clinical documentation improvement (CDI), and medical coding. The goal is to ensure that the services provided are translated into accurate codes without delay. Inaccuracies or lag time in this stage directly lead to compliance risks, underpayments, and denials. A mastered mid-cycle process ensures that clinical value is perfectly reflected in the billing data.
Back-End (Claims & Collections): From Reactive to Proactive
The back-end traditionally involves claim submission, payment posting, denial management, and patient collections. However, a mastery approach shifts this function from being reactive to proactive. It is no longer about simply “working” denials. It is about using data from every denial to perform root cause analysis, identifying patterns and fixing systemic front-end or mid-cycle issues to prevent those same denials from ever happening again.
Measuring Success: Gold-Standard KPIs for RCM Mastery in 2026
What you do not measure, you cannot improve. Moving beyond acceptable industry benchmarks to elite “mastery targets” is what separates thriving organizations from those merely surviving. Here are the gold-standard KPIs for 2026.
Days in A/R: From 40-50 to Under 30 Days
Days in Accounts Receivable (A/R) measures the average number of days it takes to collect payments due. While the industry benchmark often hovers between 40-50 days, an elite RCM process consistently operates under 30 days, dramatically improving cash flow.
Clean Claim Rate: Surpassing 98%
This KPI measures the percentage of claims submitted to payers that are processed and paid on the first pass without any errors. A standard rate is 85-90%, but mastery means achieving a Clean Claim Rate of over 98%, which signifies an exceptionally efficient front-end process.
Initial Denial Rate: Driving Below 4%
This is the percentage of claims denied upon first submission. While a rate of 5-10% is common, a high-performing RCM cycle actively drives this number below 4%. This is a direct indicator of proactive error correction and strong payer rule adherence.
Net Collection Rate: Hitting the >99% Gold Standard
This metric reflects the percentage of the allowed reimbursement that is actually collected. It is the ultimate measure of an RCM team’s effectiveness. While many aim for 95%, the mastery target is a Net Collection Rate exceeding 99%.
Cost to Collect: Ultimate Efficiency Below 2%
This KPI calculates the total cost of your RCM operations against the total collections. An industry average might be 3-4%, but leveraging technology and optimized workflows can drive this cost below 2%, directly boosting your bottom line.
The Modern Care VMA Edge: Automation & AI as the Engine of RCM

Achieving these mastery-level KPIs is no longer possible through manual effort alone. Payer complexity and labor shortages demand a smarter approach. This is where modern technology becomes the engine of your revenue cycle.
Robotic Process Automation (RPA) for Repetitive Tasks
RPA uses software “bots” to handle high-volume, rules-based tasks that consume valuable staff time. This includes claim status checks, payment posting, and eligibility verification. By automating these tasks, you free your skilled team to focus on high-value activities like complex denial analysis and payer negotiations. This is a core function where a remote medical biller can reduce claim denials by ensuring focus remains on exceptions.
Predictive Analytics to Prevent Denials Before They Happen
This is the game-changer for modern RCM. Instead of waiting for a denial, AI-powered predictive analytics tools scan claims before submission, comparing them against historical denial data and complex payer rules. The system flags claims with a high probability of denial, allowing your team to make corrections proactively and ensuring a higher Clean Claim Rate.
Generative AI for Automated Clinical Appeal Letters
When a complex clinical denial does occur, the appeals process can be incredibly time-intensive. Generative AI can now automate the creation of compelling appeal letters by scanning a patient’s medical records, identifying the specific clinical evidence required by the payer, and drafting a comprehensive, data-backed argument to overturn the denial in a fraction of the time.
Conquering Modern RCM Challenges
A forward-thinking RCM strategy must also be adaptive, ready to meet the challenges of the current regulatory and operational landscape.
“No Surprises Act” Compliance and Patient Transparency
The No Surprises Act mandates that providers give patients Good Faith Estimates (GFEs) for the cost of care. According to the American Hospital Association (AHA), transparency is a key legal and patient satisfaction driver. A modern RCM system must have the tools to generate accurate GFEs, creating a transparent financial experience that builds patient trust and streamlines collections.
Adapting to Value-Based Care Models
The industry’s shift from fee-for-service to value-based care requires RCM systems to track quality and outcome metrics alongside financial ones. Your process must be agile enough to manage bundled payments and other alternative payment models, ensuring you are compensated for the value you provide, not just the volume.
Addressing Staff Burnout with Smart Technology
RCM teams are facing unprecedented levels of burnout. The sheer volume of repetitive tasks and the frustration of dealing with denials can lead to high turnover. By implementing intelligent automation, you remove the administrative burden from your team. This allows you to upskill your staff, transforming them into data analysts and problem solvers, which directly addresses how medical virtual assistants reduce burnout in US healthcare practices.
FAQ (Frequently Asked Questions from Financial Leaders)
How do we start integrating AI into our existing RCM workflow?
Start with a process audit to identify high-volume, repetitive tasks that are ideal for RPA, such as eligibility verification. Care VMA provides an initial assessment to map automation opportunities with the highest impact.
What is the estimated ROI from RCM automation?
ROI varies, but our clients typically see a reduction in the cost to collect by up to 40-50% and an increase in the Net Collection Rate of 3-5% within the first 12 months, delivering a significant positive ROI.
Does my team need special technical skills to use your AI platform?
No. The Care VMA platform is designed with an intuitive user interface. We focus on upskilling your team to become data analysts and complex case handlers, while our technology manages the repetitive work.
Conclusion: Your Blueprint for Financial Resilience
Revenue Cycle Management Mastery in 2026 is not about working harder; it is about working smarter by harnessing technology. The goal is to stop managing denials reactively and start preventing them systematically. A finely tuned, AI-powered RCM process is the key to unlocking superior financial performance, reducing operational friction, and building a more resilient healthcare organization. Understanding how revenue cycle management impacts the financial health of private practices is the first step toward lasting stability.
Do not let revenue leakage inhibit your growth. Schedule a free RCM analysis with our specialists to see how our AI & KPI blueprint can be tailored to achieve your organization’s >99% collection target. A Medical Billing Virtual Assistant from Care VMA could be the strategic partner you need. Contact us today.

![Revenue Cycle Management (RCM) Mastery [AI & KPI Guide]](https://carevmahealth.com/wp-content/uploads/2026/03/Revenue-Cycle-Management-RCM-Mastery-1024x683.jpg)
