Disclaimer: This article is for informational purposes only and does not constitute professional IT or medical advice. Consult with a qualified healthcare technology expert for guidance specific to your practice’s needs.
Is your clinic’s EHR or EMR system implementation proving more complex and costly than anticipated? You are not alone. Many practice managers and IT leads face disrupted clinical workflows, staff who are hesitant to adapt to new technology, and persistent concerns about the security of sensitive patient data. This guide is designed to navigate you through these challenges, providing a clear framework of best practices to ensure a smooth, secure, and successful transition to a digitally optimized practice.
Effective EHR (Electronic Health Record) & EMR (Electronic Medical Record) management is the process of digitally administering patient health data to streamline operations, enhance care quality, and ensure interoperability among healthcare providers. It is the backbone of the modern, efficient medical practice.
Understanding the Fundamental Difference: EHR vs EMR
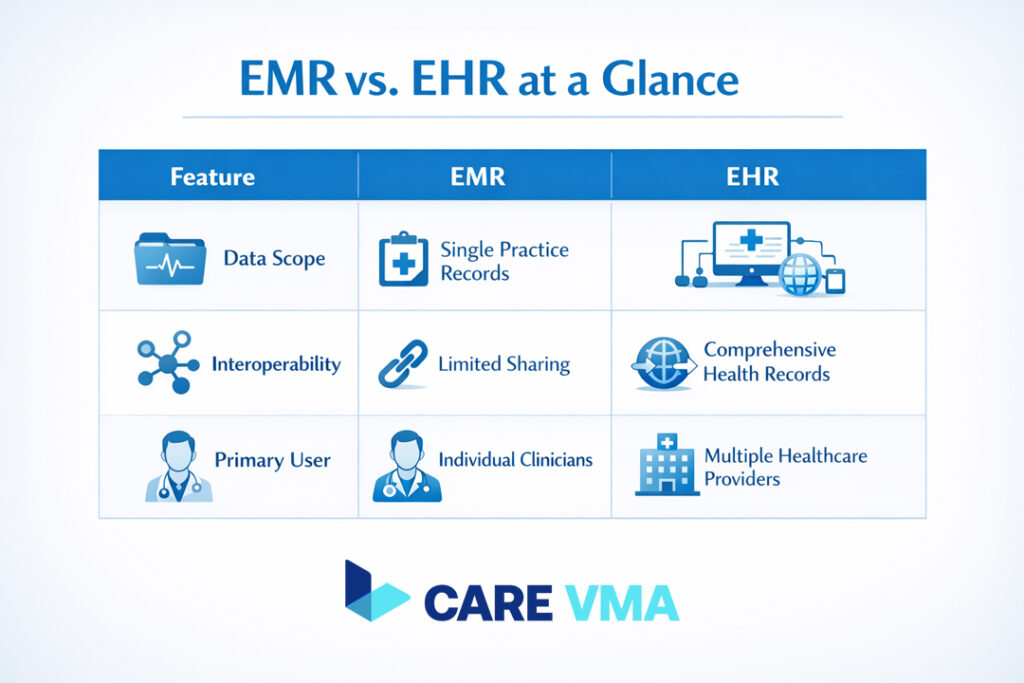
While often used interchangeably, Electronic Medical Records (EMR) and Electronic Health Records (EHR) serve different purposes. Think of an EMR as a digital version of a patient’s paper chart within a single practice. It contains their medical history, diagnoses, and treatments from one doctor or clinic.
An EHR, however, is a more comprehensive record of a patient’s overall health. It is designed to be shared across different healthcare providers, such as specialists, hospitals, and labs. The key differentiator is interoperability-the ability of different systems to communicate and share information seamlessly.
When Do You Need an EMR?
An EMR system is often sufficient for a small, standalone practice that does not frequently share patient information with outside providers. It excels at improving internal documentation, tracking patient data over time, and identifying patients due for preventive screenings within your own facility.
When is an EHR a Necessity?
An EHR is essential for any practice that coordinates care with other providers. If you refer patients to specialists, hospitals, or diagnostic centers, an EHR ensures that every provider has a complete and up-to-date picture of the patient’s health. This is crucial for improving patient safety, reducing duplicate tests, and making more informed clinical decisions.
Real-World Implementation Challenges & How to Overcome Them
Transitioning to a new digital system is a significant undertaking. Recognizing the common challenges is the first step toward creating a successful implementation strategy.
Managing High Implementation Costs
The initial investment for software, hardware, and training can be substantial. To manage this, conduct a thorough cost-benefit analysis beyond just the price tag. Factor in potential long-term savings from reduced administrative tasks, fewer medical errors, and improved billing cycles. Explore financing options or government incentives that may be available for health-tech adoption.
Overcoming Staff Resistance and the Learning Curve (The Human Factor)
The most common barrier to success is often human, not technical. Staff may be comfortable with existing workflows and resistant to change. The solution is rooted in a structured change management approach. Involve your team in the selection process, clearly communicate the benefits for their specific roles, and identify “super-users” who can champion the new system and support their peers.
Ensuring Data Security and Regulatory Compliance (HIPAA)
Protecting patient data is non-negotiable. A breach can have severe financial and reputational consequences. Ensure your chosen system is fully compliant with regulations like the Health Insurance Portability and Accountability Act (HIPAA). Implement strict access controls, data encryption, and regular security audits. Your technology partner should be able to provide clear documentation of their security protocols.
Interoperability Issues Between Systems
If your new EHR cannot communicate with the systems at the local hospital or a partner lab, its value diminishes significantly. This is a critical technical challenge. During the selection process, prioritize systems that adhere to modern interoperability standards to ensure smooth data exchange.
Avoiding Inaccurate Data Entry and “Alert Fatigue”
A system is only as good as the data within it. Inconsistent data entry can lead to clinical errors. Furthermore, many systems generate excessive notifications, leading to “alert fatigue” where important warnings are overlooked. Combat this by standardizing data entry protocols from day one and customizing alert settings to be meaningful and relevant to clinical workflows, which can be achieved by working with virtual medical assistant services.
Best Practices for Effective EHR & EMR Management [The Care VMA Framework]

A successful EHR/EMR system is not just installed; it is managed. This framework focuses on the human and process elements that are critical for long-term success.
Step 1: Needs Assessment and Strategic Planning
Before looking at any software, map your current workflows. Identify bottlenecks and specific goals. Do you need to speed up patient check-in? Improve billing accuracy? Reduce charting time for clinicians? A clear set of objectives will guide your selection and implementation process.
Step 2: Prioritizing Interoperability (HL7 & FHIR Standards)
Insist on systems that use established healthcare data standards like Health Level Seven (HL7) and Fast Healthcare Interoperability Resources (FHIR). These standards act as a universal language, allowing different healthcare systems to communicate effectively and securely. This is the cornerstone of true care coordination.
Step 3: Building a Robust Data Security Protocol
Your security plan should include more than just a strong password. Implement role-based access to ensure staff can only view the information necessary for their jobs. Enforce multi-factor authentication and have a clear data backup and disaster recovery plan in place.
Step 4: Standardizing Data Entry for Integrity
Create and enforce clear guidelines for how data is entered into the system. Use templates and dropdown menus where possible to reduce free-text variation. Consistent data is essential for accurate reporting, billing, and clinical decision-making. Proper clinic workflow optimization ensures these standards are met.
Step 5: Comprehensive Training Programs and Ongoing Support
Training should not be a one-time event. Provide initial, role-based training that focuses on the workflows each team member will use daily. Follow up with regular check-ins and offer easily accessible support resources. A well-trained team is an efficient and confident team. Providing your team with a structured program like VMA training for healthcare professionals can significantly reduce the learning curve.
Step 6: Optimizing Workflows, Not Just Digitizing Them
The goal is not to create a digital version of your old paper-based system. It is an opportunity to re-engineer and improve your processes. Work with your team to redesign workflows to take full advantage of the system’s automation and efficiency features.
Step 7: Regular System Performance Evaluation and Monitoring
After going live, regularly evaluate the system’s impact. Are you meeting the goals you set in Step 1? Gather feedback from your staff and monitor key performance indicators (KPIs) like patient wait times, billing claim denial rates, and time spent on documentation. Use this data to make continuous improvements.
Optimizing Your Practice: Management Solutions from Care VMA
Implementing these best practices can be demanding. Care VMA provides targeted support to ensure your practice maximizes the return on its technology investment.
Expert Implementation Consulting and Planning from Care VMA
Our system architects work with you to conduct a thorough needs assessment, select the right technology, and create a strategic implementation plan that minimizes disruption to your practice.
Customized Staff Training for Your Practice
We go beyond generic software manuals. Care VMA develops and delivers training programs tailored to the specific roles and workflows of your staff, accelerating adoption and ensuring proficiency.
Managed Technical Support and Data Security Services
Focus on patient care, not IT troubleshooting. Care VMA offers ongoing technical support and managed security services to ensure your system runs smoothly and your data remains protected.
FAQ (Frequently Asked Questions About EHR & EMR Management)
What is interoperability in the context of EHR, and why is it crucial?
Interoperability is the ability of different EHR systems to exchange and use patient data securely and effectively. It is crucial because it allows a doctor at a hospital to see the treatment history from a patient’s primary care clinic, ensuring seamless, coordinated care and preventing redundant tests.
How do we ensure our EHR system is compliant with regulations like HIPAA?
Ensure your vendor provides a Business Associate Agreement (BAA) and has certifications for compliance. Internally, you must implement security best practices, including role-based access controls, data encryption, and regular staff training on privacy rules. Partnering with an expert can help ensure all compliance requirements are met.
Are cloud-based systems more secure than on-premise?
Both can be highly secure if configured correctly. Modern cloud solutions often provide enterprise-grade security managed by dedicated experts, which can be more robust than what a smaller practice can manage in-house. On-premise systems give you direct control but require a strong internal IT team to handle maintenance, updates, and security monitoring.
Conclusion & Next Steps
Successful EHR and EMR management is far more than a software choice-it is a strategic initiative in change management, team training, and process optimization. While the challenges of implementation are real, they are entirely surmountable with a thoughtful, structured plan. By focusing on the human factors and prioritizing secure, interoperable technology, you can transform your practice into a more efficient, secure, and patient-centered organization.
Feeling overwhelmed by the EHR/EMR implementation process? You do not have to navigate it alone. Schedule a free consultation with our medical system architects at Care VMA to map out your path to a streamlined and secure digital practice. Explore our Virtual Medical Assistant Services to see how we can help.

![EHR & EMR Management: A Best Practice Guide [2026 Update]](https://carevmahealth.com/wp-content/uploads/2026/02/EHR-EMR-Management-1024x683.jpg)
