Claim denials are piling up, your staff is spending hours chasing down cryptic error codes, and your practice’s cash flow is slowing to a crawl. You’ve invested in practice management software, but the problem isn’t going away. Sound familiar? This isn’t just a minor administrative headache; it’s a significant drain on your revenue and your team’s morale. Each rejected claim represents a delay in payment, increased administrative costs, and, in some cases, lost revenue that you’ll never recover. Time that should be dedicated to patient care is instead lost to navigating the complex bureaucracy of insurance payers.
But what if there was a way to break this cycle? Imagine a system where claims are meticulously checked before they’re sent, your clean claim rate soars, and payments arrive faster and more predictably—all without overloading your current team.
Software & Clearinghouse Management in healthcare is the process of using a digital platform (clearinghouse) to validate, format, and electronically submit medical claims from providers (clinics) to payers (insurance). Effective management ensures claims are ‘clean’ on the first submission, drastically reducing denials and accelerating the revenue cycle (RCM). This guide is built on the analysis of thousands of claim cycles and proven best practices in Revenue Cycle Management, designed to give you a clear path forward.
What Exactly is a Healthcare Clearinghouse and Why Does Management Matter?
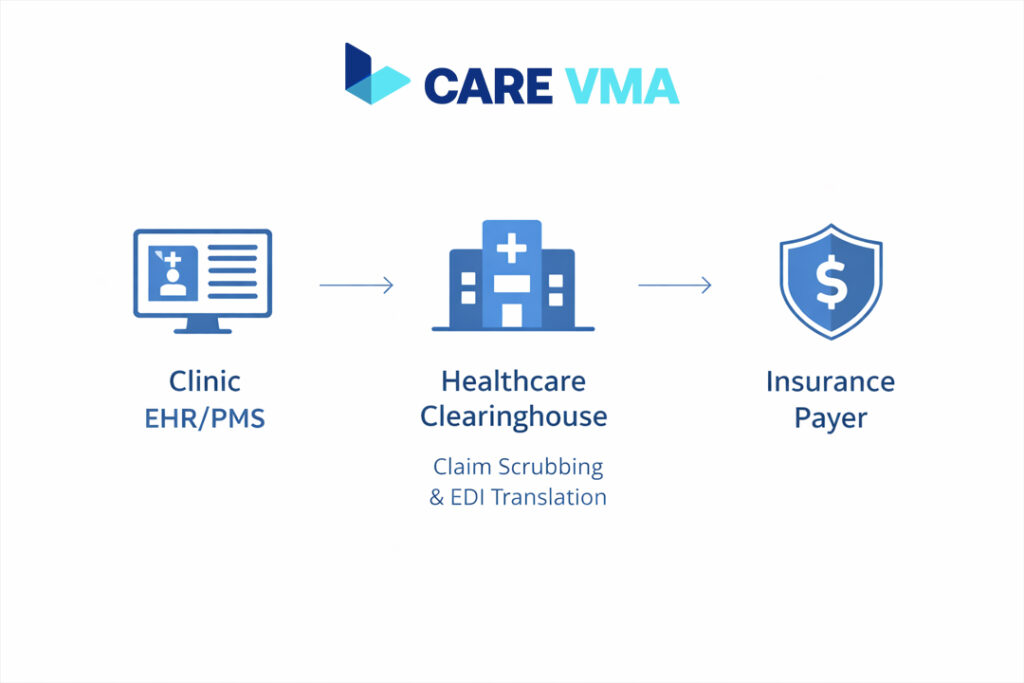
You might think of a clearinghouse as just another piece of software, but its real value lies in its role as a critical translator and gatekeeper. At its core, a Healthcare Clearinghouse acts as a central hub that bridges the gap between your clinic’s Practice Management System (PMS) and the hundreds of different insurance Payer systems, each with its own unique formatting requirements.
Here’s the thing: your PMS speaks one language, and each insurance company speaks another. The clearinghouse translates your claim data into a standardized format, known as Electronic Data Interchange (EDI), ensuring it meets strict HIPAA compliance and can be understood by the payer. It’s the essential middle step that prevents communication breakdowns.
However, simply having the software is not enough. The difference between a system that bleeds revenue and one that maximizes it comes down to active, daily management. This is where most practices fall short—they have the tool but lack the dedicated expertise to operate it effectively.
The 4 Core Functions Your Clearinghouse Process MUST Master
Mastering the daily functions of your clearinghouse is the difference between a struggling revenue cycle and a thriving one. It’s not about complex features; it’s about consistently executing four critical tasks that directly impact your bottom line.
Problem: Endless Rejections from Simple Typos & Missing Info → Solution: Automated Claim Scrubbing
It’s incredibly frustrating to have a claim denied for a simple typo in a patient’s date of birth or a missing modifier. Claim scrubbing is your first line of defense. This automated process scans every claim for errors against a vast database of payer rules before it leaves your system, catching issues with patient demographics, procedure codes, and insurance information. This single function is the key to improving your First-Pass Clean Claim Rate.
Problem: Incompatible Systems & Formats → Solution: Flawless EDI Transactions
Without a clearinghouse, your billing team would need to manually format claims for every single insurance company you work with—an impossible task. The clearinghouse handles the EDI transaction process, converting your data into the universally accepted HIPAA-compliant format. This ensures your claims are not rejected simply because they were submitted in the wrong “language.”
Problem: Denials Due to Inactive Coverage → Solution: Real-Time Eligibility Verification
One of the most preventable denials is for inactive insurance coverage. A robust clearinghouse process includes eligibility verification tools that allow your staff to check a patient’s coverage status in real-time, right at the front desk. This proactive check prevents the entire wasteful cycle of submitting a claim that was destined to be denied from the start.
Problem: Manual Payment Posting is Slow & Prone to Error → Solution: Electronic Remittance Advice (ERA) Auto-Posting
Once a claim is paid, the cycle isn’t over. Your team still needs to post that payment to the patient’s account. Manually entering this data is tedious and opens the door for errors. Electronic Remittance Advice (ERA) is the digital version of an Explanation of Benefits (EOB). Effective clearinghouse management uses ERA auto-posting to automatically apply payments and adjustments, closing the loop faster and more accurately.
Where Practices Fail: The Hidden Costs of “Unmanaged” Clearinghouse Software
What most practices don’t realize is that the biggest drain on revenue isn’t the lack of technology, but the lack of dedicated oversight. Many clinics invest in a state-of-the-art clearinghouse but fail to see a return on investment. Why? Because the system is left to run on autopilot, and critical issues are overlooked.
- Rejection Reports Are Ignored: Your clearinghouse generates daily rejection reports detailing every claim that failed the initial scrubbing process. In a busy practice, these reports often pile up, unread. Without someone analyzing these reports, you can’t identify recurring problems—like a provider credentialing issue with a specific payer—and fix them at the source.
- Vendor Management is Passive: Are you actively monitoring your clearinghouse’s performance? Do you know your average clean claim rate? Is your vendor connected to all the payers you need? Passive management means you’re likely not getting the full value from your investment and may be missing crucial updates or payer connections.
- Staff Overload & Lack of Expertise: Most front office staff and billers are already juggling multiple responsibilities. They simply don’t have the time or specialized training to become clearinghouse experts. This leads to reactive problem-solving instead of proactive management, and the cycle of denials continues.
The Solution: Expert VMA-Led Clearinghouse Management
So, if the software isn’t the problem, what’s the real solution? It’s not about replacing your tools; it’s about adding a layer of focused expertise to manage them. This is where a Care VMA Virtual Medical Assistant trained in Revenue Cycle Management becomes a game-changer. We don’t replace your software; we maximize its potential.
A dedicated VMA acts as your expert operator—the “driver” for your powerful software “car.” They bridge the gap between having the technology and getting real results.
How a Care VMA Transforms Your Process:
- Daily Rejection & Denial Management: Your VMA doesn’t just run reports; they analyze every single rejection and denial each day. They identify the root cause, whether it’s a coding error, a credentialing problem, or a payer-specific rule, then correct and resubmit the claim immediately.
- Proactive Payer & System Monitoring: Your VMA actively monitors EDI connections to ensure claims are successfully transmitted and received. They serve as the direct point of contact with your clearinghouse vendor to troubleshoot any technical issues, freeing your staff from long support calls.
- Performance Reporting That Matters: Forget overwhelming data sheets. Your VMA provides concise weekly or monthly reports highlighting the key metrics you actually care about: Clean Claim Rate, Days in A/R, and top denial trends. More importantly, these reports come with actionable recommendations for improvement.
Use Case in Action:
A busy pediatric clinic kept facing denials from Payer X for routine vaccine codes. Their in-house biller was too swamped to investigate. A Care VMA analyzed the rejection reports and discovered that Payer X required a specific modifier that wasn’t configured in the PMS. The VMA worked directly with the clearinghouse vendor to create a custom rule, permanently resolving 100% of these denials and recovering an estimated $2,500 per month in revenue.
Struggling to keep up with rejection reports and payer rules? A dedicated expert can turn your RCM process around. Discover how a Care VMA Medical Billing Assistant can take control of your clearinghouse management.
The Outcome: Higher Revenue, Lower Stress, and Better Patient Focus
The impact of expert management goes far beyond just getting claims paid. It transforms the financial and operational health of your entire practice, creating a positive ripple effect across three key areas.
- Financial Health: By systematically reducing denials and ensuring a higher clean claim rate (often up to 98% or more), your practice experiences faster, more predictable payments. This directly improves cash flow and increases net revenue.
- Operational Efficiency: Delegating the tedious, time-consuming tasks of claim management to a specialized VMA frees up your in-house staff. They can now focus on higher-value activities like improving the patient experience, managing schedules, and supporting your clinical team.
- Strategic Insight: With clear, consistent reporting from your VMA, you finally have a true understanding of your revenue cycle performance. You can make informed business decisions based on real data, not guesswork, to further optimize your practice’s financial health.
DIY Management vs VMA-Led Management: A Cost-Benefit Analysis
When considering a solution, it’s helpful to look at the numbers. Let’s break down the true cost-benefit of managing this in-house versus with a specialized VMA.
| Metric | In-House / DIY Management | Care VMA-Led Management |
|---|---|---|
| Cost | Full-time staff salary + benefits + ongoing training + cost of lost revenue from unworked denials. | A predictable, lower monthly subscription cost with no overhead. |
| Expertise | Administrative generalist juggling RCM with many other tasks. | Dedicated RCM specialist with focused training on various clearinghouses and payer rules. |
| Focus | Divided attention, tasks are often interrupted by patient-facing duties. | 100% dedicated focus on claim submission, rejection analysis, and denial follow-up. |
| Outcome | Inconsistent results, high staff burnout, persistent revenue leaks. | Measurable improvement in RCM metrics, reduced team stress, and consistent financial performance. |
To build a truly resilient revenue cycle, it’s vital to understand all its components. Mastering your clearinghouse is one part; understanding the entire system is another. Learn more about how Revenue Cycle Management impacts the financial health of private practices. For a deeper dive into preventing issues before they start, explore our guide to Denial Management and Prevention. Ultimately, the goal is to optimize every step, which is the core function of our Revenue Cycle Management Services.
FAQ: Your Top Clearinghouse Management Questions Answered
Let’s address some of the most common questions practice managers have about optimizing their clearinghouse process.
What is the difference between clearinghouse software and a clearinghouse service?
The software is the tool; the service is the expert who operates it. Software from providers like Waystar or Availity provides the digital platform. A management service, like that provided by a Care VMA, involves a trained professional performing the daily tasks—analyzing rejections, correcting claims, and monitoring performance—to ensure the tool delivers maximum financial results.
Can a VMA work with my existing EHR and clearinghouse?
Absolutely. Our Virtual Medical Assistants are trained to be platform-agnostic. They are experts at adapting to and mastering the leading EHR, PMS, and clearinghouse systems already used by medical practices. Our goal is to optimize what you have, not force you to change systems.
How do I measure the ROI of a clearinghouse management service?
The return on investment is clear and measurable. It’s calculated by (1) the increase in revenue from claims that were previously being denied or ignored, (2) the reduction in staff hours and associated costs spent on reworking claims, and (3) the improvement in cash flow from a shorter payment cycle. We provide the reports to track these exact metrics.
Take Control of Your Revenue Cycle Today
Don’t let the complexities of clearinghouse management continue to erode your practice’s profitability and burn out your team. The problem often isn’t your software—it’s the lack of dedicated, expert time to manage it day in and day out. Proactive management is the key to unlocking a healthier, more predictable revenue stream.
Ready to see how a layer of expert management can transform your practice’s financial health?


