Disclaimer: This article is intended for clinical operational improvement purposes and does not constitute medical advice.
The clinic doors close, but your workday is far from over. The real marathon begins: hours spent in front of the EHR, finishing charts, and preparing for tomorrow. This “pajama time” is a primary driver of physician burnout. Pre-charting and visit preparation is a high-efficiency workflow that moves administrative tasks out of the patient encounter and into a structured preparation phase. This strategy, endorsed by the American Medical Association (AMA) STEPS Forward program, is proven to reduce after-hours documentation time by 20-30 percent and sharpen patient focus.
The constant pressure of documentation contributes significantly to professional fatigue. Adopting new workflows can be a key part of the solution, as studies from the [National Institutes of Health (NIH)](https://www.ncbi.nlm.nih.gov/pmc/articles/PMC69529 burnout/) show the systemic nature of this issue. It’s time to reclaim your evenings by implementing a smarter, team-based system.
Distinguishing Pre-Charting vs Pre-Visit Planning
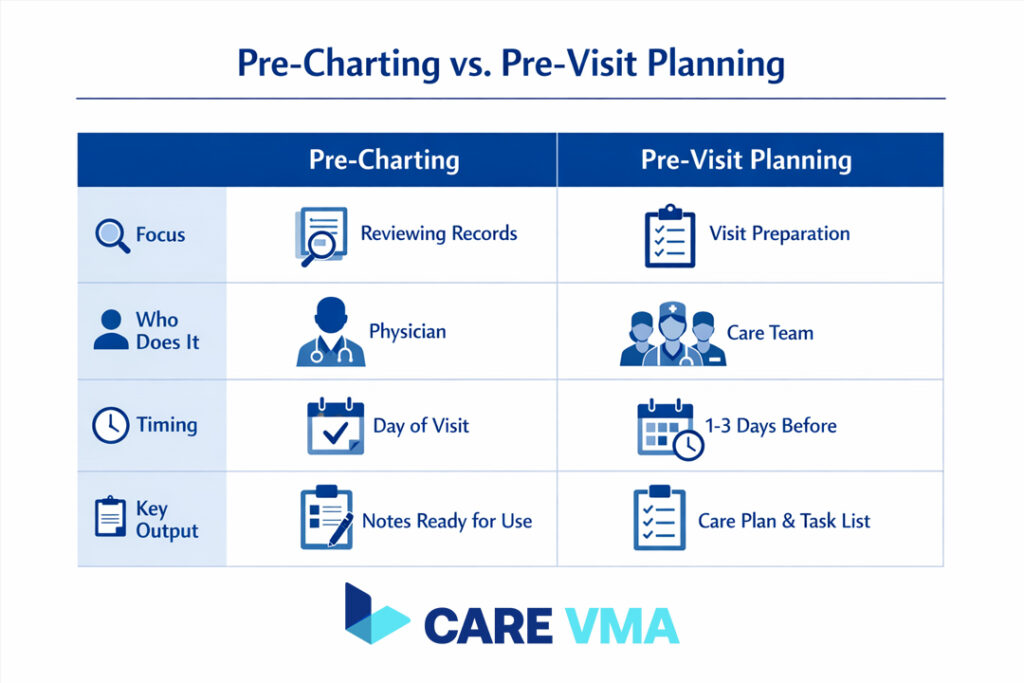
While often used interchangeably, these terms represent different scopes of work. Pre-charting is a specific task, while pre-visit planning is a comprehensive team strategy. Understanding the difference is the first step toward building an efficient clinical workflow.
Pre-Charting
- Focus: Drafting the medical note, reviewing recent data, and preparing the physician’s documentation for the encounter.
- Who Does It: Physician, Medical Scribe, or a Virtual Assistant.
- Timing: Typically 2-5 minutes right before the patient enters the room or at the start of the day.
- Key Output: A head start on the SOAP note, with HPI and relevant history pre-loaded.
Pre-Visit Planning (PVP)
- Focus: Ensuring total operational and clinical readiness for the entire patient visit, including closing care gaps.
- Who Does It: A coordinated team effort involving Medical Assistants (MAs), nurses, schedulers, and physicians.
- Timing: Starts 24-48 hours before the visit and continues through the morning huddle.
- Key Output: Lab orders completed, care gaps identified, required forms sent, and the daily schedule optimized.
The 10-Step Pre-Visit Planning Workflow (AMA STEPS Forward Model)
The American Medical Association provides a validated 10-step framework to systematize pre-visit planning. This model turns chaotic preparation into a predictable, delegable process.
Schedule the Next Visit at Check-out
The workflow begins before the current visit even ends. Secure the next appointment date before the patient leaves to ensure continuity and allow for long-range planning.
Conduct Pre-Visit Lab Testing
Order necessary labs to be completed one week before the next scheduled visit. This ensures results are available for a meaningful face-to-face discussion, eliminating frustrating follow-up calls.
“The Scrub”: Chart Cleanup 24-48 Hours Prior
A designated team member (like an MA or nurse) “scrubs” the chart 1-2 days in advance. They check for missing specialist notes, ER discharge summaries, and outstanding lab results, ensuring the chart is complete.
Identify Care Gaps
During the scrub, the team identifies and flags any overdue preventive care, such as mammograms, colonoscopies, or A1c tests for diabetic patients.
Pre-Visit Phone Call (For Complex Patients)
For patients with complex chronic conditions, a brief call from an MA can update their medication list, confirm the visit agenda, and manage expectations.
The Morning Huddle
This is a non-negotiable 10-minute daily meeting. The care team quickly reviews the day’s schedule, identifies potential bottlenecks, and assigns tasks, like ensuring a specific vaccine is ready for a patient.
Send Pre-Visit Questionnaires
Automate the dispatch of digital forms for patients to complete at home. This can include reason-for-visit forms, medication updates, or standardized screeners like the PHQ-9.
Provider Pre-Charting
With the chart scrubbed and ready, the provider can now spend a few focused minutes pre-charting. This involves reviewing the prepared information and loading a note template with the chief complaint and relevant history.
Standardized Rooming with Standing Orders
Empower MAs with standing orders to act on identified care gaps during rooming. For example, if the chart scrub noted an overdue flu shot, the MA can administer it based on protocol.
The Warm Handoff
Before the provider enters the room, the MA delivers a concise, 60-second summary of the patient’s status, their goals for the visit, and any identified care gaps.
Best Practices: Visit-Specific Preparation
A one-size-fits-all approach to preparation is inefficient. The workflow should adapt to the needs of each appointment type to maximize its impact.
Chronic Care Visits (Diabetes/Hypertension)
Preparation should focus on data tracking. Ensure the last three blood pressure readings or glucose logs are entered. Check the EHR for overdue foot exams, eye exams, or kidney function tests.
Annual Wellness Visits (AWV)
For these comprehensive visits, pre-populate Medicare-required screening tools. Verify the patient’s eligibility and have the 10-year prevention schedule ready to review for any new recommendations.
Acute/Sick Visits
Efficiency is key. Review notes from previous visits for similar complaints to see what treatments were effective. Was a specific antibiotic prescribed? Did a nebulizer treatment work? This context saves critical time.
Modern Solutions: Tools and Technology to Accelerate Preparation
Implementing this workflow manually can be challenging. Modern technology, however, makes it seamless and scalable.
AI Ambient Scribes and Pre-Visit Summaries
Tools like Freed and Nuance now offer AI-powered summaries that condense the last several encounters into a brief paragraph, allowing providers to get up to speed in seconds.
Leveraging EHR Dashboards (Epic, Cerner, Athena)
Modern EHRs have built-in “Health Maintenance” or population health dashboards. Train your team to use these visual tools to instantly spot overdue screenings and care gaps, turning a manual search into a quick glance. Good EHR-EMR management is foundational to this process.
Quick Templates (Dot Phrases / SmartPhrases)
Create EHR shortcuts for common pre-charting scenarios. A simple command like “.DIABPREP” can automatically pull the last A1c, LDL, microalbumin, and relevant notes into your template, saving minutes per chart.
Medical Virtual Assistants: Delegate Your Chart Prep
The most powerful accelerator for this workflow is delegation. A trained Virtual Medical Assistant (VMA) can perform the most time-consuming steps—chart scrubbing and care gap identification—overnight. Your team arrives in the morning to a schedule of fully prepared charts, ready for the day’s clinical tasks. This approach allows you to implement the AMA model without overburdening your current staff. The right VMA can handle many of the 10 administrative and clinical tasks that slow down your practice.
Success Tips and Overcoming Common Hurdles

Great strategy requires great execution. These practical tips help ensure your pre-visit planning workflow succeeds.
The “Blank Screen” Rule
Make it a policy to never walk into an exam room with a blank note screen. At a minimum, the chief complaint and a pre-loaded template should be ready.
Build Morning Momentum
Dedicate the first 15 minutes of the day to pre-charting the first 3-4 patients. This front-loading creates a productivity buffer that carries you through the day.
Delegate Lab Ordering with “Standing Orders”
Create protocols that empower your MAs to queue up routine labs based on the chart scrub. This prevents the provider from becoming a bottleneck for simple, recurring orders.
Handling the “No-Show” Dilemma
What happens when you prepare a chart and the patient doesn’t show up? Implement a simple rule: for patients with a high no-show history, spend no more than two minutes on pre-charting. Do the full preparation only after they have checked in.
Frequently Asked Questions
How much time can I really save?
Practices that consistently apply this model report saving 20-30% of their after-hours documentation time. For a typical physician, this translates to 30-45 minutes reclaimed every single day.
Does this method require more staff?
Not necessarily. It is primarily about restructuring the workflow of your existing team. However, to achieve maximum efficiency without adding to your in-house payroll, utilizing a Medical Virtual Assistant is an extremely cost-effective solution for handling preparatory tasks.
How do I start if my team is resistant to change?
Start small with a pilot project. Implement the full 10-step workflow for just one provider or for one day of the week. Measure the time saved and the reduction in errors, then present that data to the team to win their support.
Conclusion & Next Steps
Stop letting documentation dictate your evenings. By implementing a structured, team-based pre-visit workflow and leveraging modern technology like Virtual Medical Assistants, you can shift your focus back to where it belongs: on providing excellent patient care. This isn’t just about efficiency; it’s about restoring work-life balance and preventing the burnout that plagues modern medicine.
Tired of pajama time? Let Care VMA’s certified Virtual Medical Assistants prepare your charts overnight so you can go home on time. Schedule a free 15-minute workflow consultation today to discover how we can help you reclaim your day.

![Pre-Charting & Visit Preparation: An Efficient Workflow [AMA Model]](https://carevmahealth.com/wp-content/uploads/2026/03/Pre-Charting-Visit-Preparation-1024x683.jpg)
