Your practice delivers excellent patient care, but are you constantly battling claim denials, delayed payments, and revenue leaks you can’t seem to trace? The frustration is real. What most people don’t realize is the issue often lies in the operational gap between two critical roles that seem similar on the surface: medical coding and medical billing. One small mistake in translation by the “Coder” can lead to a complete rejection that the “Biller” has to spend hours fighting. This friction costs you time and, more importantly, money that should be in your bank account.
Medical coding is the process of translating patient encounters into universal alphanumeric codes (the ‘what’ and ‘why’), while medical billing uses those codes to create and submit claims to insurance companies to get paid. In short, coders create the clinical story; billers sell that story for reimbursement. This guide, based on an analysis of thousands of claim cycles by certified RCM specialists at Care VMA Health, breaks down the precise differences, shows how they must work together, and reveals how to turn this common point of failure into a streamlined revenue engine.
Medical Billing vs Medical Coding: At a Glance Comparison
Before we dive deep, let’s get a clear, high-level view. Understanding the core function of each role is the first step to identifying where your revenue cycle might be breaking down. The fundamental difference lies in their primary goal: accuracy versus reimbursement.
| Feature | Medical Coding (The “Translator”) | Medical Billing (The “Negotiator”) |
|---|---|---|
| Primary Goal | Clinical Data Integrity & Accuracy | Financial Reimbursement & Revenue |
| Main Task | Assigns codes (ICD-10, CPT) to diagnoses & procedures. | Creates claims, submits them to payers, and follows up. |
| Key Interactions | Physician notes, clinical documentation, EHR systems. | Insurance companies, patients, clearinghouses. |
| Core Skillset | Analytical, detail-oriented, knowledge of anatomy. | Communicative, persistent, organized. |
| Key Tools | Code books (digital/physical), encoder software, EHR. | RCM/Billing software, insurance portals, CMS-1500 form. |
What is Medical Coding? The “Translator” of Patient Care
Think of medical coding as the foundation of your entire revenue cycle. If this foundation has cracks, the whole structure is at risk of collapse. The coder’s job isn’t just administrative; it’s a highly technical task of translating every aspect of a patient encounter into a universally understood language.
A certified medical coder meticulously reviews a provider’s documentation within the Electronic Health Record (EHR)—from physician’s notes to lab results. They then assign the correct codes from systems like the International Classification of Diseases (ICD-10-CM) for diagnoses and the Current Procedural Terminology (CPT) for procedures and services. Their work is all about accuracy and data integrity.
For example, a patient visit for ‘Type 2 Diabetes’ (Diagnosis) with a ‘flu shot’ (Service) is translated by the coder into specific, billable codes like E11.9 and 90686. Without these exact codes, the story of the visit is incomplete for the payer, leading to an immediate query or denial.
Key skills for a medical coder include:
- An almost obsessive attention to detail.
- A strong analytical mindset to interpret clinical documentation.
- Deep knowledge of medical terminology, anatomy, and physiology.

What is Medical Billing? The “Negotiator” for Reimbursement
If coders write the story, billers are the ones who ensure that story has a profitable ending. Here’s how they turn codes into cash flow. The medical biller takes the clean, coded data and uses it to formally request payment from an insurance payer. Their job is about navigating the complex financial side of healthcare.
The biller’s workflow begins where the coder’s ends. They take the assigned codes (like E11.9 and 90686) and create a formal invoice, typically on a CMS-1500 form. This claim is then submitted electronically to the insurance company. But their job doesn’t stop there. They are responsible for the entire journey of that claim, including:
- Tracking the claim status.
- Posting payments received from the payer.
- Investigating, appealing, and resolving any claim denial.
- Billing the patient for their portion (co-pays, deductibles).
Continuing our example: The biller submits the claim with the E11.9 and 90686 codes. If the insurer denies it, citing ‘lack of medical necessity,’ the biller becomes the practice’s financial advocate. They investigate the denial reason, communicate with the payer, and may need to file a formal appeal to secure the payment your practice has earned, all while adhering to HIPAA regulations.
Key skills for a medical biller include:
- Excellent communication and negotiation skills.
- Persistence and tenacity to follow up on denied claims.
- Strong organizational abilities to manage dozens or hundreds of claims at once.
Where the System Breaks: The Critical (and Costly) Gap Between Billing and Coding 🔥
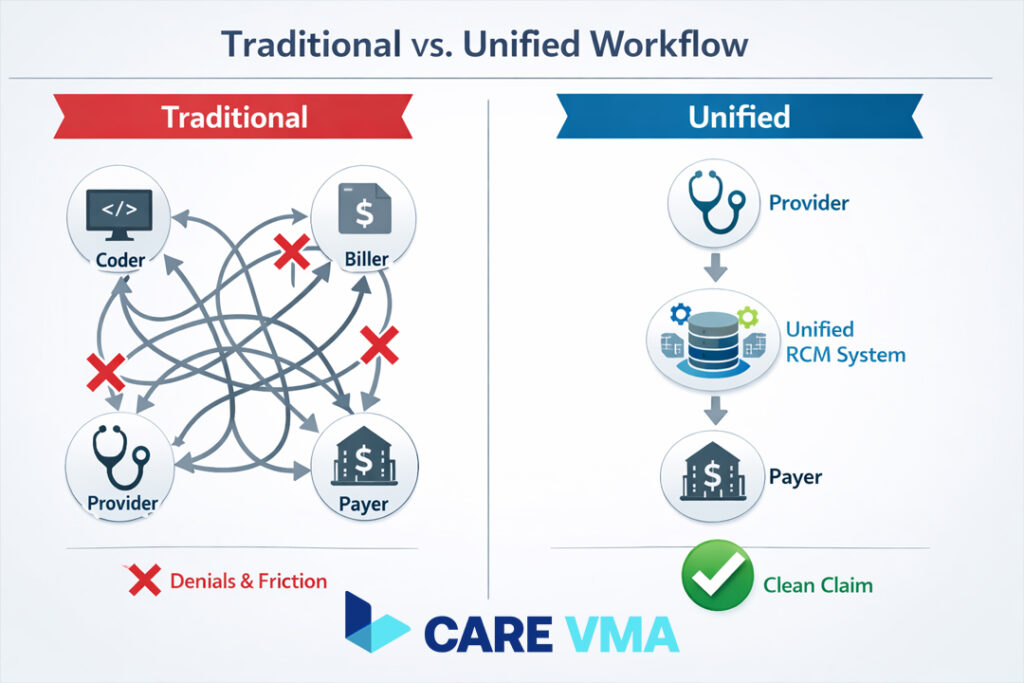
Here’s the part most guides skip, and it’s likely where your practice is losing the most money. The real issue isn’t what coders and billers do in isolation, but how they fail to work as an integrated system. When these two roles operate in separate silos, revenue leakage is inevitable.
What does this breakdown look like in practice?
- A coder, under pressure, uses a non-specific diagnosis code. The biller submits the claim, and it’s instantly denied for lack of specificity. The biller now has to chase down the coder and physician, wasting hours of everyone’s time.
- A biller doesn’t understand why a specific coding modifier was used, so they remove it before submission. The claim gets paid, but the practice is underpaid by 20-50% for that service.
- Worst of all, there is no feedback loop. The biller sees a trend of denials from a specific payer for a certain procedure, but that information never gets back to the coder who could prevent the error from happening in the first place. This is how small errors become chronic, costly problems.
Industry data shows that up to 80% of medical bills contain errors, and a significant portion of these originate from coding inaccuracies or the disconnect between the coding and billing process. For a small practice, this can easily translate to tens of thousands in lost revenue annually. This is a problem that requires a systematic, not just a personnel, solution for effective denial management and prevention.
Does this cycle of coding errors leading to billing fires sound familiar? An integrated approach can break this costly pattern. Learn how a virtual medical billing assistant can help.
Unifying Your Revenue Cycle: The Care VMA Advantage
Fixing a fractured system isn’t about telling people to ‘communicate more.’ It’s about giving them the tools and workflows that make seamless integration the default. This is where a modern, unified approach to Revenue Cycle Management (RCM) becomes a game-changer.
Instead of seeing coding and billing as a hand-off, Care VMA treats it as a single, cohesive ecosystem. Our platform and trained virtual assistants directly solve the costly gap:
- Reduces Errors Proactively: Our AI-driven system and expert staff can cross-reference codes against specific payer rules before a claim is ever submitted. This flags potential errors for coders, preventing the denial before it even happens and drastically improving your medical coding accuracy.
- Creates a Powerful Feedback Loop: When a denial occurs, the reason is automatically tracked and analyzed. This data provides immediate, actionable insights to the coding team, creating a continuous improvement loop that strengthens your entire revenue cycle month after month.
- Increases Team Efficiency: Instead of operating in separate software or spreadsheets, your billing and coding functions are unified. This eliminates manual data re-entry, streamlines communication, and gives you a single source of truth for your practice’s financial health.
In-House vs Outsourced: Which Model is Right for Your Practice?
Now that you understand the system, the next big question for a practice manager is: who should run it? The answer has significant implications for your budget, control, and long-term growth.
In-House Team
- Pros: You have maximum control over daily processes and staff priorities. The team is fully integrated into your practice culture.
- Cons: This is often the most expensive model. It involves high overhead for salaries, benefits, training, and software. You’re also responsible for managing staff turnover, vacations, and ongoing education to keep up with coding changes.
Outsourcing with a Partner (like Care VMA)
- Pros: You gain immediate access to a team of certified experts without the hiring and training costs. Costs are predictable, and you eliminate the headaches of staff management. It allows your core team to focus on patient care.
- Cons: You have less direct, minute-to-minute oversight of the team’s process.
What most practices find is that framing it as “outsourcing” is misleading. With Care VMA, you’re not just handing off a task; you’re gaining a strategic partner whose entire focus is dedicated to maximizing your financial health.
FAQ (Frequently Asked Questions)
Let’s tackle some of the most common questions practice managers have about these two critical roles.
What is the main difference between medical billing and medical coding?
Medical coding involves translating clinical services, diagnoses, and procedures into universal alphanumeric codes. It’s about data accuracy. Medical billing uses these codes to create and submit claims to insurance companies for financial reimbursement. It’s about getting paid.
Can a person do both medical billing and coding?
Yes, absolutely. In smaller practices, it’s common for one person to handle both roles. Professionals certified in both are highly versatile, though the roles require different primary skillsets—analytical for coding and communicative for billing. Leading certification bodies like the American Academy of Professional Coders (AAPC) offer credentials for both.
Which is more difficult, medical billing or coding?
“Difficulty” is subjective and depends on an individual’s skills. Medical coding is technically complex, requiring a deep understanding of anatomy and thousands of codes governed by strict rules. Medical billing is administratively complex, requiring persistence, attention to detail, and strong negotiation skills to deal with insurance payers.
Your Revenue Cycle is a System, Not a Checklist
It’s time to stop treating medical billing and coding as two separate administrative tasks. They are the two most critical components of a single, interconnected revenue system. The financial health and stability of your practice depend entirely on the seamless flow of information between the “Translator” (the coder) and the “Negotiator” (the biller). Optimizing that link is the single most powerful lever you can pull to increase revenue, reduce administrative waste, and allow you to focus more on what truly matters: your patients.
Ready to see what a unified system can do for your bottom line? Don’t let operational gaps and preventable errors continue to drain your practice’s resources.
Stop letting claim denials dictate your revenue. See exactly how much hidden revenue Care VMA can unlock for your practice. Schedule a free, no-obligation RCM analysis with one of our specialists today.


