Medical Disclaimer: The information in this article is for informational purposes only and does not constitute medical advice. It is not a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of a qualified health provider with any questions you may have regarding a medical condition.
Have you or your clinical team ever felt the intense anxiety of waiting for lab results that seem to have vanished into thin air? A single lost or delayed result can stall a crucial diagnosis, postpone essential treatment, and erode patient trust. This is an unnecessary and dangerous risk in modern healthcare. The solution is a ‘closed-loop’ diagnostic coordination system, an integrated framework designed to eliminate these gaps and ensure every test is accounted for, from order to action. Lab and diagnostic coordination is the systematic management of laboratory and imaging services that ensures every test is ordered, processed, delivered, and clinically acted upon in a secure, unbroken workflow.
Why Fragmented Diagnostic Coordination is a High-Risk Gamble?

A disconnected diagnostic process is not just inefficient; it is a significant threat to patient safety and a drain on resources. When communication between the clinic, the lab, and the patient breaks down, the consequences can be severe. Studies have shown that a lack of coordinated follow-up can have profound impacts.
Risk of Diagnostic Errors and Treatment Delays
The most critical risk is a missed or delayed diagnosis. According to the Centers for Disease Control and Prevention (CDC), a substantial portion of diagnostic errors can be traced back to failures in the testing process, including ordering, reporting, and follow-up. When an abnormal result is not communicated effectively, a patient’s condition can worsen, leading to more complex and costly interventions down the line.
Cost Inefficiencies from Redundant Testing
When a test result is lost, the most common response is to order a repeat test. This not only doubles the cost but also consumes valuable staff time and patient effort. A fragmented system lacks a single source of truth, making it difficult for providers to confirm if a test was ever completed, leading to unnecessary duplication and straining healthcare budgets.
Psychological Impact on Patients: Anxiety and Eroding Trust
For patients, the waiting period for test results is already a stressful experience. When that period is extended by administrative errors or lost information, it can cause significant anxiety and fear. This experience can damage the patient-provider relationship, leading to a loss of trust in the healthcare facility’s competence and care.
Anatomy of a ‘Closed-Loop’ System: How It Actually Works
A ‘closed-loop’ system transforms this fragmented process into a secure, transparent, and accountable workflow. It operates on a simple principle: every diagnostic test ordered must be verifiably acknowledged, resulted, and followed up on. This is achieved through four distinct phases.
Pre-Analytic Phase: From Test Order to Sample Collection
This phase begins the moment a clinician orders a test within the Electronic Health Record (EHR). The system immediately logs the order, handles any necessary prior authorizations, and provides the patient with clear instructions for sample collection or scheduling. This eliminates manual data entry errors and ensures all prerequisites are met before the sample is even collected.
Analytic Phase: Focusing on Turnaround Time (TAT) and Quality Control
Once the sample arrives at the lab, it is tracked by a Laboratory Information System (LIS). The focus here is on efficient and accurate processing. The ‘closed-loop’ system monitors the Turnaround Time (TAT) against established benchmarks, flagging any delays for immediate attention. This phase is governed by strict quality standards, such as those from CLIA and CAP, to ensure result accuracy.
Post-Analytic Phase: Integrating Results into the EHR and Critical Notifications
After analysis, the results are automatically transmitted from the LIS directly into the patient’s EHR. This seamless integration is the core of the system. There is no manual transcription, which is a major source of error. The system is programmed to identify and flag critical or abnormal results, sending instant alerts to the ordering physician and care team to ensure urgent issues are addressed immediately. Efficient EHR/EMR management is the backbone of this critical step.
Clinical Follow-Up Phase: Closing the Loop with Patient Action
The loop is not closed until the provider has reviewed the results and a clear follow-up action has been taken and documented. This could be scheduling a follow-up appointment, prescribing medication, or simply communicating the results to the patient. The system tracks this final step, ensuring no result is left unaddressed.
The Team Behind the System: Key Roles in Modern Diagnostic Coordination
A robust technological framework requires skilled professionals to manage it. Unlike older, siloed models, a modern diagnostic system relies on specialized roles to ensure the seamless flow of information and care.
Diagnostic Coordinator: The Frontline for Order Tracking and Authorization
This individual acts as the central point of contact for all diagnostic tests. They are responsible for tracking orders from placement to completion, managing insurance prior authorizations, and proactively addressing any logistical hurdles. They ensure that patients complete their tests and that results are routed to the correct provider, often serving as a key part of a virtual patient care coordinator team.
LIS Coordinator: The Guardian of Data Flow Between Lab and EHR
This is a more technical role focused on maintaining the integrity of the data pipeline. The LIS Coordinator ensures that the laboratory information system and the electronic health record are communicating flawlessly. They troubleshoot integration issues, manage system updates, and are essential for preventing the data loss that plagues less advanced systems.
Diagnostic Management Team (DMT): The Strategic Brain for Complex Cases
A DMT is a multidisciplinary group, often including pathologists, radiologists, and clinicians, that collaborates on complex or unusual cases. By reviewing diagnostic strategies together, they ensure that testing is both clinically appropriate and cost-effective, providing a layer of expert oversight that improves diagnostic accuracy and patient outcomes.
The Care VMA Solution: Integrated Technology to Close the Gaps
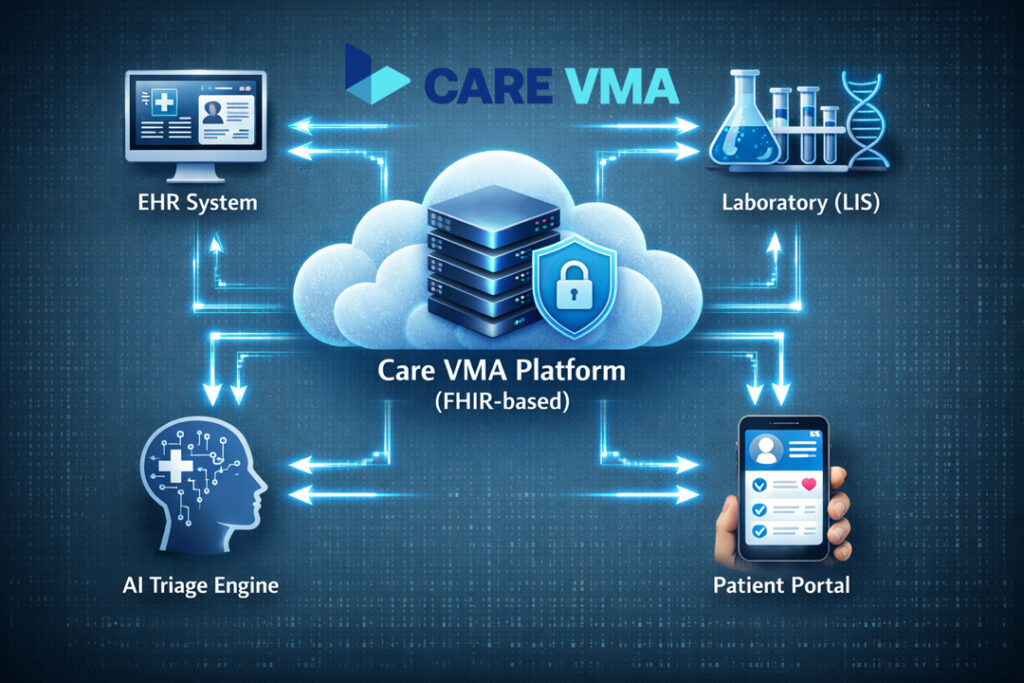
At Care VMA, we leverage cutting-edge technology to build and support these ‘closed-loop’ systems, converting diagnostic uncertainty into operational certainty. Our solutions are designed to address the core challenges of interoperability and human error head-on.
LIS and EHR Integration with FHIR Standards: Breaking Down Information Silos
The biggest challenge in health tech has always been getting different systems to communicate. We use modern data standards like FHIR (Fast Healthcare Interoperability Resources), which allows disparate systems like your LIS and EHR to speak the same language. This eliminates data silos and creates a unified, real-time view of the patient’s diagnostic journey.
AI-Powered Results Triage: Ensuring Critical Results Are Never Missed
Human oversight can lead to delays, especially in high-volume environments. Our systems can incorporate AI-driven triage tools that automatically scan incoming results, identify critical values, and prioritize them for clinician review. This intelligent automation acts as a digital safety net, ensuring the most urgent cases get immediate attention and helps address the root causes of physician burnout solutions by reducing cognitive load.
Unified Patient Portals: Empowering Patients with Access and Understanding
A truly closed loop must include the patient. We facilitate the integration of patient portals that provide patients with direct, timely access to their lab results. Paired with clear, easy-to-understand explanations, this empowers patients to become active participants in their own care and is a powerful tool for improving patient engagement.
FAQ (Frequently Asked Questions for Clinics and Facilities)
How does the Care VMA system ensure my patient data is secure and HIPAA compliant?
We use end-to-end encryption and a platform that is fully compliant with HIPAA security standards to guarantee the confidentiality and integrity of all patient data at every step of the process.
Can this service integrate with my hospital or clinic’s existing systems?
Yes. Our platform is built on modern interoperability standards like HL7 and FHIR, allowing it to communicate and integrate with the vast majority of existing EHR and LIS systems.
What is the first step if I want to use Care VMA’s diagnostic coordination services?
The first step is to schedule a brief consultation with our team. We will map out your current workflow, identify key points of friction, and demonstrate exactly how our platform can optimize your diagnostic processes.
Conclusion & Next Steps
Adopting a ‘closed-loop’ diagnostic coordination system is no longer just an option for forward-thinking clinics; it is a fundamental requirement for ensuring patient safety, achieving operational efficiency, and providing peace of mind. By bridging the gaps where critical information can get lost, you create a more resilient and reliable healthcare experience for everyone involved.
Do not let essential diagnostic results fall through the cracks of a complex system. Contact the experts at Care VMA today. Let us show you how our Virtual Patient Care Coordinator services can help you build a secure, efficient, and fully integrated workflow for your practice.


