Provider credentialing is the process of verifying a healthcare provider’s qualifications, training, and professional history to ensure they meet industry standards. Payer enrollment is the subsequent process of contracting with insurance networks (like Medicare, Medicaid, and commercial payers) to become eligible for reimbursement for services rendered. This two-part system is the gateway to your practice’s revenue, but for many, it feels more like a roadblock.
A new provider is ready to see patients, but your practice is losing thousands each week because they aren’t enrolled with payers. Claim denials are piling up due to small administrative errors, and your team is buried in follow-up calls and paperwork.
Here’s the thing: this 150-day waiting game isn’t just frustrating; it actively drains your cash flow, burns out your staff, and jeopardizes your practice’s financial health. Every single delay is money you can’t reinvest in patient care or practice growth. But there is a systematic, expert-led approach to cut this timeline dramatically and ensure you get paid for every service, starting from day one. This process is fully aligned with the latest 2026 standards from the National Committee for Quality Assurance (NCQA) and CMS.
The Vicious Cycle: How Flawed Credentialing & Enrollment Kills Your Revenue
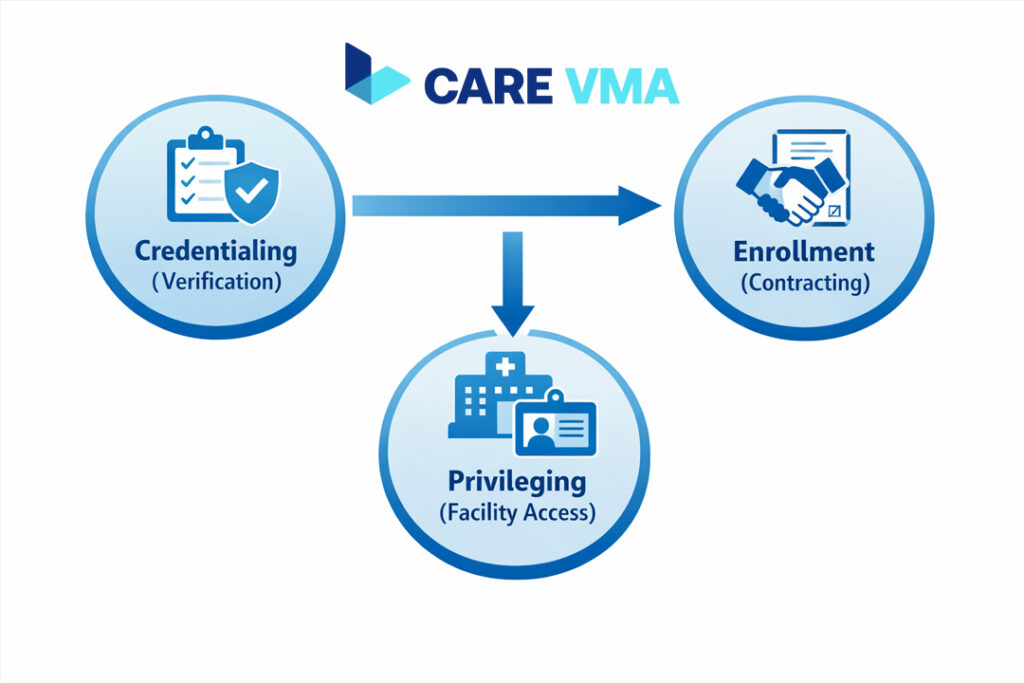
At first glance, the terms seem interchangeable. But understanding the distinction is the first step to fixing the financial leaks in your practice. What most people don’t realize is that these are three separate, sequential processes, and a failure in one creates a domino effect of delays.
- Credentialing: This is the foundational “professional background check.” It involves Primary Source Verification (PSV) of every qualification—from medical degrees and board certifications to state licenses and DEA registration.
- Enrollment: This is the “contracting” phase. Once a provider is verified, you must enroll them with each individual insurance network, both government (Medicare/Medicaid via the PECOS system) and commercial. This is what makes a provider “in-network” and eligible for payment.
- Privileging: This step is specific to facilities like hospitals or ambulatory surgery centers. It grants a provider permission to perform specific procedures within that facility based on their proven competence.
Each step depends on the one before it. You can’t enroll a provider who hasn’t been credentialed, and you can’t get paid until they are enrolled. This complex relationship is where bottlenecks form, leading directly to lost income.
The Top 5 Credentialing Mistakes Costing Your Practice Over $100,000
Feeling like you’re stuck in an endless loop of paperwork and follow-up calls? You’re not alone. These administrative hurdles aren’t just annoyances; they have a real, calculable financial impact. Here are the top five errors that quietly siphon revenue from your practice.
The 150-Day Black Hole: Delays in Payer Applications
The single biggest source of revenue loss is the gap between a provider’s start date and their credentialing effective date with payers. An average 120 to 150-day delay for a provider who generates $1,500/day in services translates to a staggering $180,000 to $225,000 in lost or delayed revenue. This isn’t just a delay; it’s a massive hit to your cash flow.
The “Gap Trap”: Unexplained Work History Gaps That Trigger Rejection
Payers are meticulous. Any unexplained gap in a provider’s CV or work history, often as short as 30 days, can trigger an immediate rejection of the application, sending you back to square one. What seems like a minor oversight forces your team to track down the provider, get a written explanation, and restart the entire submission process, adding weeks or even months to the delay.
The Silent Killer: Expired Licenses & Lapsed CAQH Re-attestations
In the world of credentialing, maintenance is everything. A lapsed state license, an expired malpractice insurance policy, or a failure to perform the quarterly CAQH re-attestation can bring the entire process to a halt. The CAQH ProView profile is a central hub for payers, and if it’s not meticulously maintained, applications will be frozen, leading to surprise claim denials months later.
The Wrong Date: Seeing Patients Before the Payer’s “Effective Date”
This is a painful and entirely preventable mistake. A provider might be credentialed and approved, but if they see patients before the official “effective date” on their contract with a specific health plan network, those claims will be denied. The payer has no obligation to reimburse for services rendered before they officially consider the provider in-network, turning rendered care into pro-bono work.
The Document Maze: Missing or Incorrectly Formatted Paperwork
Each payer has its own unique set of requirements. Submitting an application without the correct attachments, using an outdated form, or missing a signature is the fastest way to get your file sent to the bottom of the pile. This lack of a standardized process creates a maze of administrative work that is highly prone to human error, causing friction and costly delays.
The Complete 2026 Credentialing & Enrollment Playbook: A Step-by-Step Guide
To win the credentialing game, you need a proactive strategy, not a reactive one. The key is to think of it as a 150-day project plan that begins long before your new provider is scheduled to see their first patient.
Pro-Tip: Start the entire process 120-150 days before the provider’s anticipated start date.
NCQA 2026 Update Alert: New standards now require stricter monthly monitoring of exclusion lists and license expirations. This shift from periodic checks to ongoing vigilance makes a manual, spreadsheet-based approach riskier than ever. According to the NCQA, this is critical for maintaining patient safety and compliance.
Phase 1: The Credentialing Phase (Verification – Days 1-45)
- [ ] Day 1: Collect all required documents from the provider. This is your master file and should include everything: CV, state licenses, DEA, board certifications, malpractice insurance face sheet, and their National Provider Identifier (NPI) number.
- [ ] Day 5: Begin Primary Source Verification (PSV). Contact every institution directly to verify the documents are authentic.
- [ ] Day 10: Update or create the provider’s CAQH ProView profile. Ensure every single section is complete and the provider has performed their re-attestation.
- [ ] Day 20: Internally audit the complete file. Check for work history gaps, mismatched dates, or missing information. Get explanations for any gaps now.
- [ ] Day 45: Present the clean, verified file to your internal credentialing committee for approval.
Phase 2: The Enrollment Phase (Contracting – Days 46-120+)
- [ ] Day 46: Immediately upon internal approval, begin submitting applications to your top 5-10 payers, starting with Medicare and Medicaid.
- [ ] Day 55: Begin aggressive, weekly follow-up with every payer. Document every call: who you spoke to, the date, and the status of the application. Do not wait for them to contact you.
- [ ] Day 90: Review submitted contracts. Pay close attention to the proposed fee schedule and, most importantly, the requested effective date.
- [ ] Day 120+: Receive the executed contract and confirmation of the provider’s effective date. Communicate this date clearly to your scheduling and billing teams.
This checklist provides a framework, but the real challenge lies in the execution—the hundreds of follow-up actions and meticulous tracking required for every provider and every payer.
Stop Chasing Paperwork: The Modern Solution to End Revenue Loss
This is where many practices hit a wall. The administrative burden of this process is immense, and it pulls your skilled staff away from patient-facing activities. This is why forward-thinking practices reframe the problem. Instead of asking “How do we do this cheaper?”, they ask, “How do we turn this cost center into a revenue accelerator?”
This is where a strategic partner like Care VMA comes in. We integrate specialized virtual assistants directly into your workflow, transforming the administrative maze into a streamlined, predictable system.
How Care VMA Solves Your Top Credentialing Problems:
- We Eliminate the Waiting Game: Our team takes over 100% of the aggressive follow-up with payers. We know who to call, what to ask, and how to escalate issues to get applications processed faster. We transform 150 days of uncertainty into a predictable workflow, directly impacting your bottom line. An organized approach to insurance verification and prior authorization is a core part of this process.
- We Eradicate Administrative Burden: Forget juggling dozens of spreadsheets. Our virtual assistants become the single source of truth for all provider documents, applications, and statuses. They manage the CAQH profiles and set automated alerts for expiring licenses, ensuring nothing falls through the cracks.
- We Prevent Denials Before They Happen: Our internal audit process is meticulous. Before any application is sent to a payer, we ensure it’s 100% accurate and complete. This pre-emptive quality control leads to a first-pass submission success rate of over 98%, directly preventing claim denials related to credentialing issues.
Real-World Impact:
A multi-specialty clinic hired three new providers set to start in the same quarter. By handling the process internally, they projected a revenue loss of over $90,000 due to standard enrollment delays. After partnering with Care VMA, all three providers were successfully enrolled and seeing patients within 75 days, cutting the projected revenue loss in half and accelerating their time-to-payment by nearly 50%.
The Tangible Outcomes: Faster Payments, Less Stress, Better Care
Partnering with a specialist isn’t just about offloading a task; it’s about achieving better business outcomes that allow you to focus on your primary mission: patient care.
- Accelerated Cash Flow: Start receiving payments for your new providers’ services in 60-90 days, not 150+. This drastically improves your practice’s financial health.
- Reduced Administrative Waste: Reclaim up to 25 hours of valuable staff time per provider, per month. That’s time your team can re-invest in patient scheduling, engagement, and improving the in-office experience.
- Bulletproof Compliance: Gain peace of mind knowing that ongoing monitoring for licenses, DEA registrations, and sanctions is handled systematically, keeping you aligned with the latest NCQA standards for 2026.
- Focus on Patient Growth: Shift your energy from administrative fires to strategic initiatives. Expand your services, market your new providers, and grow your practice, knowing the revenue cycle is secured.
DIY Credentialing vs Partnering with a Specialist
When you factor in staff time and, most critically, lost revenue from delays, the “true cost” of handling credentialing in-house becomes clear.
| Feature | In-House / DIY | Care VMA Specialist |
|---|---|---|
| Time to Revenue | 120-150+ days | Avg. 60-90 days |
| Staff Time | 20-30 hours/provider | <2 hours/provider (for data) |
| Denial Risk | High (due to common errors) | Minimal (<2% rate) |
| Ongoing Monitoring | Manual, prone to error | Automated & Guaranteed |
| True Cost | Staff Salary + Lost Revenue | Fixed, Predictable Fee |
Explore Further Resources
Understanding how credentialing fits into the bigger picture is key to optimizing your practice.
- To see how this process impacts your entire financial ecosystem, read our guide on how Revenue Cycle Management impacts the financial health of private practices.
- For a deeper dive into the foundational steps, review our article that offers a clear explanation of medical credentialing.
- Learn how a virtual medical admin assistant can become an essential partner in streamlining these and other crucial tasks.
Frequently Asked Questions
What is the difference between provider credentialing and provider enrollment?
Credentialing is the verification of a provider’s qualifications (like a background check). Enrollment is the process of getting that provider contracted with an insurance company so they can get paid. Credentialing must be completed before enrollment can begin.
How long does provider credentialing take?
The entire process, including enrollment, typically takes 90 to 150 days. Delays are common and can be caused by missing information, slow payer responses, or errors in the application. A strategic approach can often reduce this to 60-90 days.
What is CAQH and why is it important?
CAQH is a central online database where providers store their credentialing information. Insurance companies use it to streamline the process, but the provider’s data must be kept updated and re-attested every 90-120 days to remain active and prevent application delays.
Conclusion: Stop Waiting, Start Earning
Stop letting cumbersome administrative processes dictate your practice’s revenue and timeline. The delays, denials, and administrative burnout associated with provider credentialing and enrollment are not a cost of doing business—they are a sign of a flawed system. By implementing a proactive, expert-driven strategy, you can transform this bottleneck from a source of frustration into an accelerator for your revenue cycle.
Ready to stop the waiting game? Download our free Provider Credentialing & Revenue Loss Checklist to identify the critical gaps in your current process.
Or, skip the trial-and-error. Schedule a Free 15-Minute Consultation with a Care VMA specialist. We will analyze your current workflow and provide you with actionable steps to get your providers paid faster. No risk, no obligation—just a clear path to reclaiming your lost revenue.

![Expert Provider Credentialing & Enrollment [Get Paid Faster]](https://carevmahealth.com/wp-content/uploads/2026/03/Expert-Provider-Credentialing-Enrollment-1024x683.jpg)
