Your practice is busier than ever. You’re managing more patients with chronic conditions, dealing with staff shortages, and fighting administrative burnout. You’ve heard about Remote Patient Monitoring (RPM), but the last thing you need is another complex system for your team to manage. What if you could improve patient outcomes and generate over $1,200 per patient annually, without adding to your team’s workload? This is how.
Remote Patient Monitoring (RPM) uses digital technology to collect patient health data, like blood pressure and glucose levels, from outside the clinical setting. For healthcare practices, the primary benefits are improved clinical outcomes, significant new revenue streams, and greater operational efficiency. This guide explains how to move beyond theory and implement a successful RPM program that enhances care while reducing administrative burden.
The Core Benefits of RPM: A Four-Pillar Framework for Your Practice
Implementing any new service can feel daunting. The key is to understand its impact across your entire practice. We’ve broken down the benefits of RPM into a simple, four-pillar framework: Financial Growth, Clinical Excellence, Operational Efficiency, and Strategic Positioning. Each pillar represents a critical area of your practice that RPM can fundamentally improve—when operationalized correctly.
Pillar 1: Financial Growth & Sustainable Revenue
“RPM is a well-reimbursed service, but how do you capture that revenue without creating a billing nightmare?”
This is where most practices hesitate. The promise of new revenue is enticing, but the fear of complex billing rules and time-tracking burdens can halt progress. A successful RPM program isn’t just about the technology; it’s about the workflow that supports reimbursement.
Unlocking New Revenue with RPM CPT Codes
Medicare and many private payers reimburse for RPM services through a set of specific CPT codes. Think of these not as confusing regulations, but as billable actions that create a predictable monthly revenue stream.
- CPT 99453: A one-time payment for the initial device setup and patient education.
- CPT 99454: A monthly payment for supplying the device and monitoring daily data transmission.
- CPT 99457 & 99458: Monthly, time-based payments for care management, data analysis, and patient interaction.
The challenge isn’t knowing the codes; it’s meticulously documenting the work to justify them. This is where a Virtual Medical Assistant (VMA) transforms RPM from a logistical headache into a seamless profit center.
The VMA Billing Workflow in Action
- Patient Setup (CPT 99453): Your VMA handles the entire remote onboarding process. They educate the patient on using their cellular-enabled device, confirm the first data transmission, and document the encounter. This ensures the claim for 99453 is valid and audit-proof from day one.
- Monthly Monitoring (CPT 99454): To bill this code, you need at least 16 days of readings per month. Your VMA monitors a centralized dashboard for compliance, proactively contacting patients who miss readings to keep them on track. This simple step guarantees you meet the requirement for 99454 every month.
- Care Management (CPT 99457): This is where most revenue is lost due to poor time tracking. Your VMA performs the initial data review and triage. They document every minute spent on patient communication, data analysis, and care coordination. Once 20 minutes are accrued, the VMA prepares the report for billing 99457, making the entire process frictionless for your staff.
Pillar 2: Clinical Excellence & Proactive Care
“Every provider wants to prevent emergencies, but who has the time to watch patient data 24/7?”
The greatest clinical benefit of RPM is the shift from reactive, episodic care to proactive, continuous intervention. Instead of relying on a single data point from a visit every few months, you get a clear view of a patient’s health in their real-world environment.
The results are staggering. The University of Pittsburgh Medical Center (UPMC) reported a 76% reduction in hospital readmissions, and a study from the Department of Veterans Affairs found that RPM programs lowered mortality rates by over 40%.
This is only possible with a system that can filter the noise and deliver actionable alerts to your clinical team.
The VMA Clinical Triage Workflow
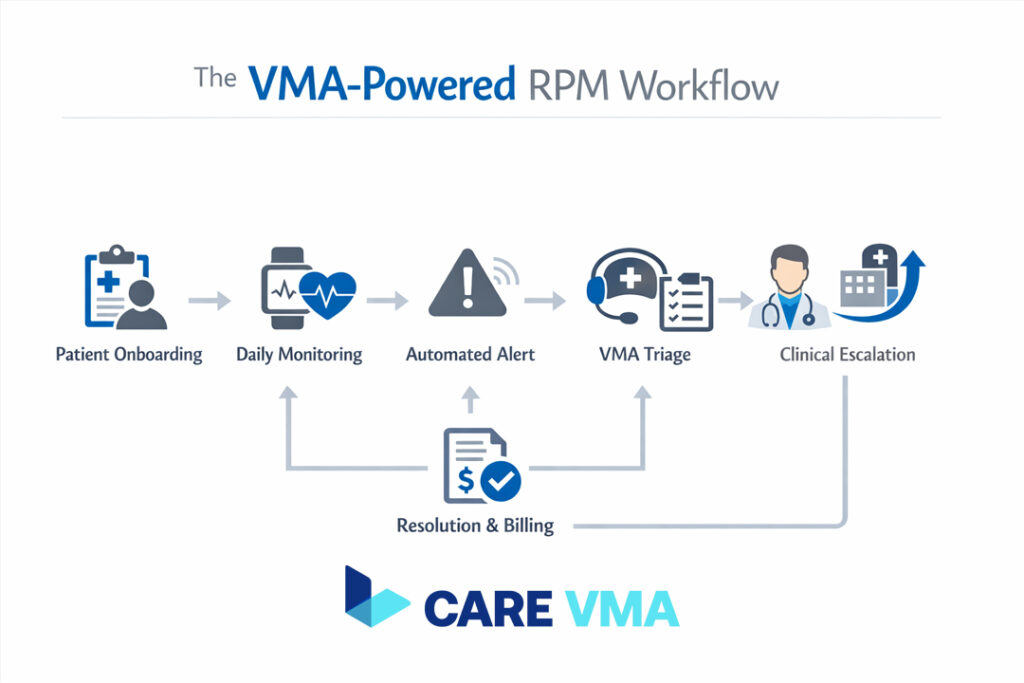
Imagine a heart failure patient whose weight, monitored by a cellular scale, increases by 3 lbs overnight—a potential sign of fluid retention.
- Automated Alert: The RPM platform instantly flags the abnormal reading and creates a high-priority alert.
- VMA Triage (First Response): Your assigned VMA is the first responder. They access the patient’s chart, review the alert against your practice’s pre-set clinical protocols, and initiate a check-in call. The VMA asks scripted questions about symptoms like shortness of breath or ankle swelling.
- Clinical Escalation: The VMA doesn’t make clinical judgments. Instead, they summarize the findings into a concise, actionable summary and send it via secure message to the designated RN or MA: “Mr. Smith (HF patient) gained 3.2 lbs overnight. Reports mild ankle swelling, no SOB. Vitals otherwise stable. Please advise.”
- Informed Resolution: Your nurse, armed with all the necessary data, can now make a quick, effective clinical decision (e.g., “Advise Mr. Smith to take his prescribed PRN diuretic and re-weigh in the morning”). The entire interaction is documented by the VMA for care management and billing purposes. Your clinical team’s expertise is used for seconds, not minutes of data gathering.
Pillar 3: Operational Efficiency & Reduced Admin Burden
“How can we possibly monitor dozens of patients remotely when our staff can barely keep up with in-office demands?”
This is the central fear for any practice manager. The solution lies in understanding that 90% of RPM work is administrative, not clinical. By delegating these tasks, you don’t just add a new service; you create new efficiencies across your entire practice. A healthcare virtual assistant is the key to offloading this work.
A Day in the Life with a VMA-Powered RPM Program
- Morning Huddle (5 Minutes): Your clinical team doesn’t log into a complex RPM portal. Instead, they review a simple dashboard prepared by the VMA, highlighting only the 2-3 patients who require clinical attention that day.
- During the Day (VMA at Work): While your in-office staff manages patients, your VMA is handling the routine RPM tasks: checking patient compliance, sending educational reminders, and documenting stable readings. No clinical staff time is used for these essential but non-clinical activities.
- Phone Calls (Reduced by up to 63%): Studies show that RPM significantly reduces the time clinicians spend on the phone. Instead of nurses making “just checking in” calls, the VMA handles these routine interactions, freeing up your clinical team for high-value work.
- Seamless EHR Integration: A VMA ensures that all RPM data, patient notes, and billable time are logged correctly and flow directly into your EHR. This eliminates the dreaded double-entry and keeps your patient charts accurate and up-to-date.
Pillar 4: Strategic Positioning for Value-Based Care
“As reimbursement shifts from volume to value, how do you prove your practice is delivering superior outcomes?”
Remote Patient Monitoring is no longer just an innovative add-on; it is becoming a foundational tool for success in modern healthcare. It directly supports the goals of value-based care by reducing hospitalizations, improving quality metrics (like HgbA1c control), and significantly enhancing the patient experience.
With patient satisfaction rates reported as high as 97%, RPM is also a powerful patient retention tool.
Using VMA-Collected Data for Population Health
Your VMA can help generate powerful reports from your RPM data. Imagine being able to show a payer that “75% of our hypertensive patients in the virtual chronic care management program are now within their target BP range.” This is the kind of objective, outcome-driven data that strengthens your position in Accountable Care Organizations (ACOs) and during payer negotiations.
The RPM Implementation Challenge vs The VMA-Powered Solution
The benefits are clear, but the implementation hurdles are real. Here’s a direct comparison of the operational challenges of a DIY approach versus a VMA-powered solution.
| The Challenge (Doing It Yourself) | The Care VMA Solution |
|---|---|
| Who handles patient training & tech support? Your already busy MAs have to add it to their overflowing schedule. | Your dedicated VMA handles all remote patient onboarding and provides ongoing tech support, ensuring patient compliance. |
| Who monitors daily readings? A nurse or MA has to manually check a portal, taking time away from other critical patient duties. | Your VMA monitors a centralized dashboard and only escalates clinically relevant alerts according to your protocols. |
| How is billable time tracked? Staff must manually log every call and minute spent, leading to inconsistent tracking and missed revenue. | Our platform automatically tracks time, and your VMA ensures every billable interaction is meticulously documented. |
| Who manages device logistics? Your office manager is now a shipping and receiving clerk, dealing with inventory and troubleshooting. | We handle all device procurement, kitting, and direct-to-patient shipping, making the process invisible to your practice. |
Overwhelmed by the “Challenge” column? That’s precisely why we built the solution. See how our VMA service works.
Frequently Asked Questions (FAQ)
How much time does an RPM program take from my clinical staff?
With a VMA, minimal. Your clinical staff’s involvement is reduced to just a few minutes per escalated alert, allowing them to focus solely on making clinical decisions.
What if my patients aren’t tech-savvy?
This is a common concern that we have solved. We use pre-configured cellular devices that work right out of the box—no Wi-Fi, apps, or smartphones are needed. Our VMAs are experts in patient education and provide support for all technology comfort levels.
Is this process HIPAA compliant?
Absolutely. The Care VMA platform, all communications, and every VMA are fully trained and operate within a secure, HIPAA-compliant framework. Patient data security is our highest priority.
How does this integrate with our current EHR?
Our system is designed for seamless integration. We work with your practice to ensure that RPM data, VMA notes, and billing reports are pushed directly into your patient charts, eliminating manual re-entry and streamlining your workflow.
Ready to Turn RPM Benefits into Your Practice’s Reality?
You’ve seen the financial, clinical, and operational benefits of Remote Patient Monitoring. More importantly, you’ve seen the operational workflow that makes it all possible without burning out your team. RPM isn’t just another piece of technology—it’s your path to a more efficient, proactive, and profitable practice.
Stop just reading about the benefits. Start realizing them. Schedule a free, no-obligation consultation with our workflow specialists today. We’ll build a custom ROI projection for your practice and show you exactly how a Virtual Medical Assistant can handle the heavy lifting.


