Inbound referral coordination is the critical process of managing patient referrals received from external providers. It encompasses every step from initial intake and insurance verification to patient scheduling and closing the loop with the referring physician, ensuring no patient falls through the cracks. For many practices, this system is broken, leading to significant patient leakage and revenue loss. The challenges discussed here are based on operational analyses of hundreds of U.S. medical practices and are supported by industry data on the pervasive issue of referral leakage.
The stack of referral faxes on your desk seems to grow overnight. Your best administrative staff spend their days playing phone tag with patients and chasing down missing clinical information from referring offices. You know patients are getting lost in the shuffle, but there’s simply not enough time or staff to manage the flood.
Here’s the thing: Every lost referral isn’t just a number in a report; it’s a direct hit to your practice’s revenue, a strain on your relationship with referring physicians, and a risk to patient care. The administrative burnout it causes is costing you your best people. But what if you could capture every single referral, schedule patients in hours instead of days, and free your team to focus on in-office patient care—all without a costly and disruptive EMR overhaul?
The Four Critical Stages of the Inbound Referral Process
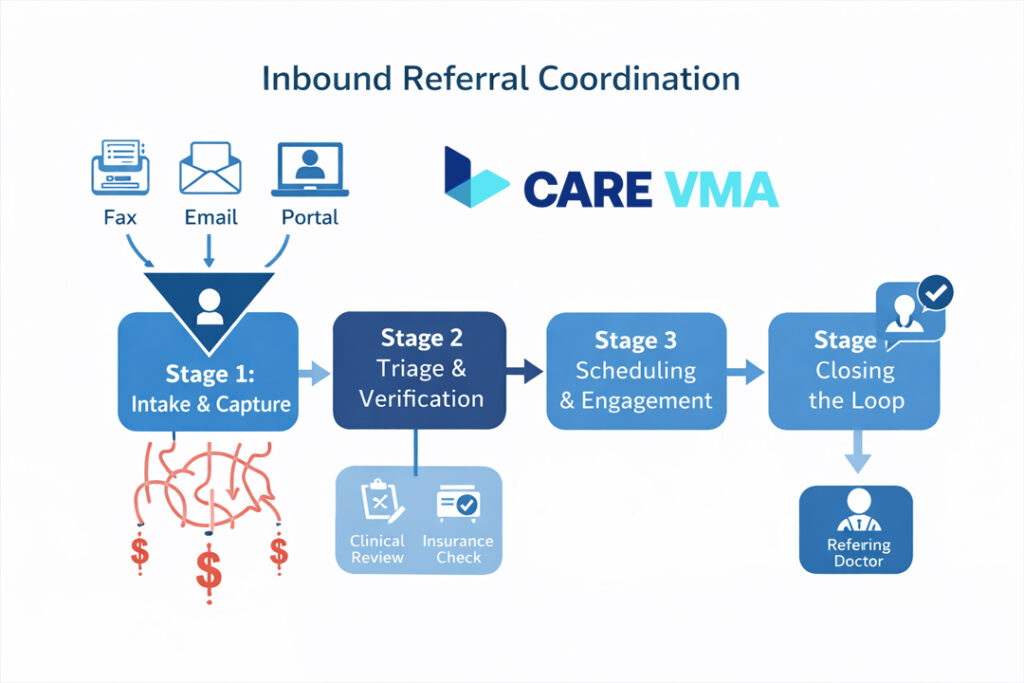
At first glance, managing referrals might seem like a simple administrative task. But in reality, a seamless and effective process requires four distinct, critical stages. Understanding this “gold standard” is the first step to identifying exactly where your own workflow is breaking down.
- Stage 1: Intake & Capture: This is the starting line. Referrals arrive from multiple channels—fax, email, your EMR portal, or phone calls. The goal is to capture every single one and centralize them into a single, manageable queue, preventing them from getting lost in a paper shuffle or a forgotten inbox.
- Stage 2: Triage & Verification: Once captured, each referral must be triaged. A coordinator reviews the attached clinical records for urgency and appropriateness. This stage involves the crucial, often time-consuming work of verifying patient demographics and running insurance verification to confirm coverage for your specialty.
- Stage 3: Scheduling & Engagement: This is where most practices lose patients. It involves proactive patient outreach to schedule their first appointment. Speed is critical; the longer the delay, the higher the chance the patient will seek care elsewhere or give up on the process entirely.
- Stage 4: Closing the Loop: After the patient is scheduled (or if the referral is declined), the final step is to communicate this status back to the referring provider. This simple act of closing the loop is fundamental to maintaining trust and ensuring a steady stream of future referrals.
Why Your Current Referral Process is Leaking 35-50% of Patients
If you feel like you’re working harder than ever but your patient volume isn’t reflecting it, you’re not imagining things. Most standard, manual referral processes are riddled with bottlenecks that actively push patients and revenue out the door. These aren’t just minor inefficiencies; they are systemic failures with significant consequences.
Manual Bottlenecks: The 25-Minute Per-Referral Trap
What most people don’t realize is the sheer amount of time a single faxed referral consumes. From deciphering handwriting and manually typing patient demographics into your EHR to checking insurance portals, staff can easily spend 25 minutes or more per referral. When you receive dozens a day, this “Fax Machine Black Hole” creates an instant backlog, delaying patient contact by days and causing staff immense frustration.
Communication Gaps: Leaving Referring Physicians in the Dark
Referring providers are the lifeblood of any specialty practice. Yet, when they send a patient your way and hear nothing back, it erodes their confidence. They don’t know if the patient was contacted, if they scheduled, or if their clinical notes were even received. When referring providers go silent, it’s often because they’ve moved on to a competitor who makes the process easier and more transparent.
Fragmented Systems: Juggling Faxes, Phones, and Your EHR
Your front office team is likely navigating a maze of disconnected systems. They receive a fax, look up the patient in the EHR, open a separate web browser for the insurance portal, and then use the phone to call the patient. This constant toggling between platforms is not only inefficient but also a major source of data entry errors and a significant contributor to administrative burden.
Delayed First Contact: Losing Patients to Competitors Before You Even Call
In today’s on-demand world, patients expect a quick response. When it takes your overwhelmed staff three to five days to make that first call, that patient has already had time to search for other options, ask friends for recommendations, or simply lose the motivation to follow through. The endless game of phone tag that follows only makes the problem worse, leading directly to lost consultations.
The Hidden Costs of a Broken Referral System
The frustration and daily chaos of a broken referral system are just the surface. Beneath the operational headaches are tangible costs that directly impact your practice’s financial health, staff stability, and long-term growth prospects.
Financial Cost: The Alarming Price of Patient Leakage
Let’s quantify the damage. Industry data consistently shows that practices lose between 35-50% of their referrals due to process failures. For a moderately busy specialty practice, this can translate to a loss of tens of thousands of dollars in billable services every single month. This isn’t just lost opportunity; it’s revenue you earned but failed to capture.
Staffing Cost: The Revolving Door of Burnout
Your referral coordinators are on the front lines of this broken process, and it’s taking a toll. High-volume, low-reward tasks lead directly to staff burnout, disengagement, and ultimately, high turnover. According to a study published by the National Institutes of Health (NIH), burnout is a significant problem in healthcare administration. The cost to recruit, hire, and train a new coordinator is substantial, and the cycle repeats itself if the underlying process isn’t fixed.
Reputational Cost: Damaging Your Most Valuable Asset
Your relationships with referring physicians are one of your most valuable assets. When their patients report delays and a lack of communication, it directly reflects on your practice. Becoming known as “difficult to work with” can permanently damage your reputation and cause your primary source of new patients to dry up.
Is Your Practice Feeling the Strain of Manual Referral Management?
If these challenges sound familiar, you’re not alone. But continuing to rely on an outdated process is no longer sustainable. It’s time to consider a modern solution that eliminates these burdens without adding new complexities.
The Modern Solution: A Human Touch Powered by Efficiency
Many practices believe they have only two options: hire more in-house staff (which is expensive and hard to scale) or buy complex new referral management software (which requires costly implementation and staff retraining). There is a third, more effective way: pairing human expertise with your existing technology.
This is where a dedicated service using highly trained Virtual Medical Assistants (VMAs) changes the game. It’s not about replacing your team; it’s about empowering them by delegating the entire administrative referral workflow.
Beyond Automation: Expert Handling of Complex Cases
Purely automated software often fails when it encounters a hurdle—an illegible fax, a non-standard insurance plan, or a missing referring provider signature. Our HIPAA-trained VMAs are experts at navigating these exceptions. They don’t just process data; they investigate incomplete referrals, perform complex insurance verification, and communicate with patients with the empathy and professionalism that an AI bot cannot replicate.
Slash Administrative Burden by 80%
Imagine your staff’s day if they didn’t have to touch a single referral fax. Care VMA’s service takes over the entire workflow. Our VMAs handle the fax intake, data extraction, and patient data entry directly into your EMR or Practice Management system. They then perform the patient outreach calls to get the appointment scheduled. Your in-house team is freed up to manage high-value tasks and provide excellent in-person patient care.
Seamless Integration, No New Software
One of the biggest barriers to improving operations is the fear of a massive technology change. Our VMA service eliminates this completely. We don’t sell you software. Our VMAs are trained to work within your existing systems—your EHR, your PM, and your phone lines. There is no disruptive migration, no new logins to remember, and no steep learning curve for your team.
Use Case: A multi-physician cardiology practice in Texas was struggling with a 3-day average delay from referral receipt to first patient contact. After delegating their inbound coordination to a Care VMA, this was reduced to under 4 hours. Within 60 days, they captured 30% more scheduled appointments from the same referral volume and saw their patient no-show rate drop by 15%.

Tangible Outcomes of Optimized Inbound Referral Coordination
Moving to an expertly managed referral process isn’t just about making your office run smoother. It’s about driving measurable results that strengthen the entire practice, from revenue to staff morale.
Increase Patient Volume and Boost Practice Revenue
By capturing the 35-50% of referrals that were previously lost, you directly increase the number of new patient appointments on your schedule. Every referral converted into a billable consultation is revenue that goes straight to your bottom line, funding growth and investment in better patient care.
Improve Staff Morale and Reduce Turnover
When you remove the most frustrating, repetitive administrative tasks from your team’s plate, you transform their work experience. They are no longer bogged down by the “work about work.” Instead, they can focus on meaningful patient interactions and higher-level responsibilities, which is a key factor in job satisfaction and retention, as noted by healthcare management resources like the World Health Organization (WHO).
Strengthen Referrer Loyalty and Secure Your Pipeline
When you make the referral process fast, transparent, and easy for referring providers, you become their preferred specialist. They will send you more patients because they trust that their patients will be cared for promptly and that they will be kept in the loop. This creates a reliable and growing pipeline of new business for your practice.
Getting Started with Care VMA
We’ve designed our onboarding to be simple, secure, and fast, ensuring a smooth transition with no disruption to your daily operations.
- Free Process Assessment: We start by analyzing your current referral workflow to identify key bottlenecks and quantify your potential for improvement.
- Match with a Dedicated VMA: Based on your needs, we match you with a dedicated, HIPAA-trained Virtual Medical Assistant who becomes an extension of your team.
- Secure Onboarding & Integration: We securely integrate with your systems and train your VMA on your specific protocols, EMR, and practice culture.
- Go-Live & Optimize: Your VMA begins managing your inbound referrals. We provide continuous oversight and performance metrics to ensure we’re meeting and exceeding your goals.
Learn More About Optimizing Your Practice Operations
Fixing your referral process is a major step toward a more efficient and profitable practice. To continue improving your operations, explore these related resources:
- Discover how a broken workflow impacts your team: Is Staff Burnout Silently Costing Your Practice? (Here’s How to Fix It)
- Tackle another common source of lost revenue: The Ultimate Guide to Reducing Patient No-Show Rates
- See our full service offering: Explore Our Full Inbound Referral Coordination Service
Frequently Asked Questions (People Also Ask Optimization)
What does a referral coordinator do?
A referral coordinator manages the entire patient referral lifecycle. Their responsibilities include receiving and processing referral documents, verifying patient insurance, scheduling appointments, and ensuring seamless communication between the referring and specialty practices to guarantee continuity of care.
How do you track inbound referrals effectively?
Effective tracking involves centralizing all referrals (from fax, phone, and EMR portals) into a single system or dashboard. Key metrics to monitor include time-to-first-contact, referral-to-appointment conversion rate, and referral volume by source. A dedicated service like Care VMA uses these metrics to eliminate leakage and optimize the process.
Are Virtual Medical Assistants (VMAs) HIPAA compliant?
Yes, absolutely. Reputable VMA services ensure their assistants are fully trained on HIPAA regulations. At Care VMA Health, all our VMAs undergo rigorous, ongoing HIPAA training and operate under strict security protocols and a signed Business Associate Agreement (BAA) to protect all patient data.
Stop Leaking Patients, Start Growing Your Practice
Stop letting a broken, outdated process dictate your practice’s growth and your staff’s sanity. The constant stress of managing manual referrals is a choice, not a necessity. By shifting from administrative chaos to a streamlined, expert-managed system, you can capture lost revenue, build stronger referrer relationships, and finally allow your talented team to refocus on what truly matters: delivering exceptional patient care.
Tired of seeing faxes pile up and revenue walk out the door? See how a dedicated Virtual Medical Assistant can transform your inbound referral process in under 30 days.
Book a Free, No-Obligation Referral Process Assessment Today. Discover exactly where your practice is leaking patients and get a customized plan to fix it.


