Patient engagement and retention are the series of strategies and technologies healthcare providers use to actively involve patients in their care and ensure they remain loyal to the practice. This is critically important in modern Value-Based Care (VBC) models to reduce patient churn, improve clinical outcomes, and boost profitability.
Is your practice losing 5-10% of its patients every year? That translates to tens, if not hundreds, of thousands of dollars in lost revenue. The frustrating part? It’s likely not due to the quality of your medical care, but because of operational issues like endless phone queues and clunky scheduling—what we call “phone friction.”
Here’s the thing: acquiring a new patient costs five times more than keeping an existing one. Every patient who walks away takes their lifetime revenue potential straight to your competitor. In 2026, the solution isn’t just about buying more software. It’s about having a smart implementation strategy that creates a seamless, proactive patient experience. This guide, based on 2026 industry trend analysis and insights from leaders like Health Catalyst, will show you exactly how.
Why Patient Retention is The New Growth Engine in Value-Based Care?
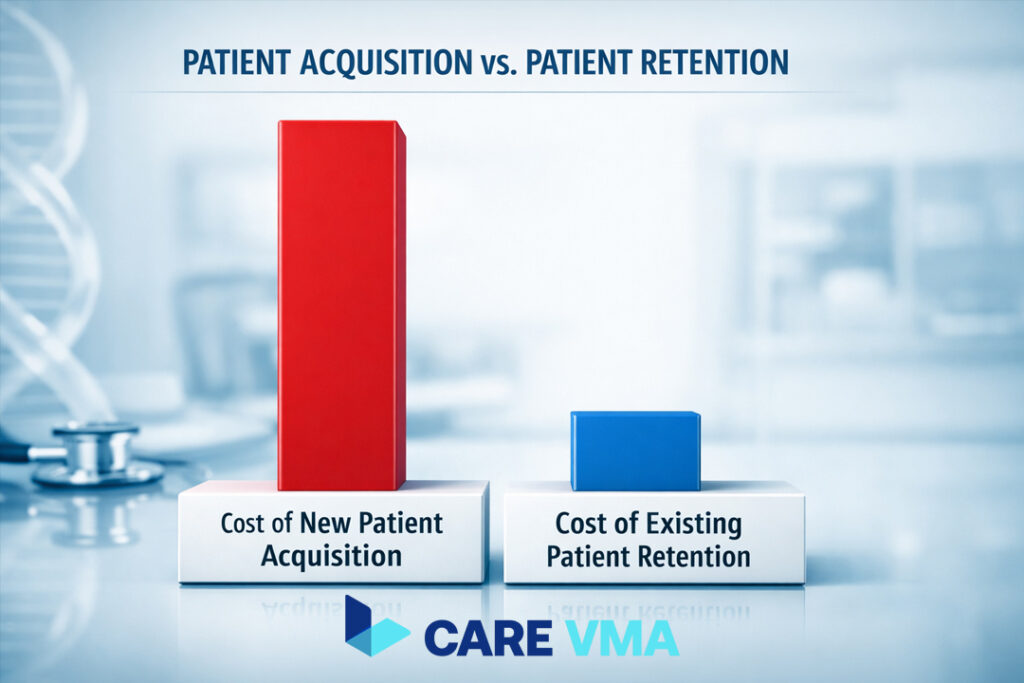
At first glance, retaining patients seems like common sense. But in today’s healthcare landscape, it’s a fundamental financial strategy. The industry is rapidly moving away from fee-for-service and toward Value-Based Care (VBC), a model where profitability is directly tied to patient outcomes and long-term wellness.
In a VBC world, keeping patients healthy and within your practice’s ecosystem isn’t just good practice—it’s the primary engine for growth. This shift coincides with the rise of Healthcare Consumerism. Patients now have service expectations shaped by on-demand industries like Amazon and Uber. They expect convenience, transparency, and personalization. If their experience is filled with friction, they won’t hesitate to switch providers, leading to increased patient churn and a direct hit to your bottom line.
The Silent Killers of Patient Loyalty: 3 Critical Challenges in 2026
What most people don’t realize is that practices often lose patients over issues that seem small but create massive frustration. These operational bottlenecks are the silent killers of loyalty and a major driver of clinician burnout.
“Phone Friction”: The #1 Reason Patients Leave
A study cited by Artera found that nearly 47% of patients are frustrated by outdated phone systems. Does your staff spend most of their day fielding scheduling calls while other critical tasks pile up? Long hold times, dropped calls, and the inability to easily reschedule create a terrible first impression and are often the final straw that sends a patient looking elsewhere. This is the biggest leak in your revenue bucket.
The Experience Gap: When Care Feels Disconnected After a Visit
Excellent in-person care can be completely undermined by a lack of follow-up. When patients leave your office and hear nothing until their next appointment, it creates an experience gap. This lack of continuity of care makes them feel like a number, not a person. Simple post-discharge check-ins or reminders for follow-up actions can make all the difference, yet they are often missed due to staff overload.
Staff Burnout & Operational Overload
The two problems above create a vicious cycle that lands directly on your staff. When administrative teams are overwhelmed with phone calls and manual follow-ups, they can’t provide the high-touch, empathetic service patients expect. This operational overload leads to mistakes, poor patient satisfaction, and ultimately, staff burnout, which only worsens the patient experience.
4 Core Strategies for World-Class Patient Engagement & Retention
To combat these challenges, leading practices are moving beyond reactive care and embracing proactive, technology-enabled strategies. It’s about meeting patients where they are and making healthcare feel effortless.
Hyper-Personalization
This goes far beyond using a patient’s first name in an email. True hyper-personalization in healthcare uses data from the Electronic Health Records (EHR) to deliver tailored communication. This includes everything from customized medication reminders based on their specific prescription to proactive outreach after a procedure, guided by their medical history. Generative AI in healthcare is making this possible at scale.
The “Digital Front Door”
Your practice’s “digital front door” is the online equivalent of your reception desk. A modern digital front door includes:
- Online self-scheduling that patients can access 24/7.
- Digital pre-registration forms to reduce waiting room time.
- “Smart waitlists” that automatically offer newly opened appointment slots to patients via SMS.
Omnichannel Communication
Patients want to communicate on their terms. A robust omnichannel communication in healthcare strategy means being available via two-way SMS, a secure patient portal, and email. The key is allowing patients to choose their preferred channel. As research shows, an overwhelming 76% of patients now want two-way, AI-driven text messaging for scheduling and payments, a statistic highlighted by Curogram.
Proactive Continuity of Care
Don’t let the conversation end when the patient leaves. Proactive continuity of care involves using automation and remote technologies to stay connected. This includes:
- Automated follow-up messages checking on their recovery.
- Supporting patients with Remote Patient Monitoring (RPM) programs.
- Scheduling brief virtual check-ins via telemedicine to ensure treatment plans are on track.
The VMA Advantage: Implementing Retention Strategies Without The Overhead 🔥
This all sounds great, but it leads to the billion-dollar question: who is going to do all of this? Buying new software for RPM or an AI chatbot creates another problem: it adds a significant operational burden on your existing staff. This is the conversion gap most tech companies ignore.
Here’s the truth: technology is only a tool. You need a trained operator to make it work.
This is the Care VMA advantage. We don’t just sell you a platform; we provide the expert human touch to run it. Our Virtual Medical Assistants (VMAs) are the “implementors” who turn these world-class strategies into reality, without adding to your overhead or causing more staff burnout.
A VMA from Care VMA closes the operational gaps by:
- Eliminating “Phone Friction”: Our VMAs handle inbound calls, manage appointment scheduling, and respond to text messages, instantly freeing your front desk from being tied to the phone. This directly impacts your no-show rate.
- Executing Omnichannel Communication: A VMA manages your SMS campaigns, sends personalized email follow-ups, and monitors the patient portal, ensuring no patient message is missed.
- Supporting Your RPM & CCM Programs: VMAs can monitor basic RPM data, escalate anomalies to your clinical team, schedule telehealth check-ins, and manage your chronic care management workflows, ensuring these valuable programs run smoothly.
- Boosting Practice Efficiency: Our VMAs proactively manage your smart waitlist, filling canceled slots in real-time.
For example, an orthopedic clinic used a Care VMA to manage their surgical waitlist. When a last-minute cancellation occurred, the VMA immediately contacted the next patients via SMS. They successfully filled 90% of empty slots in under an hour—a task impossible for a busy front desk staff.

Key Metrics to Prove Your Retention Strategy is Working
How do you know if your efforts are paying off? Shifting to a retention-focused model requires tracking the right metrics. This isn’t just about feeling busier; it’s about measurable improvement.
- Patient Retention Rate: The most direct measure. It’s the percentage of patients from a specific time period who return for another visit within a defined window (e.g., 18-24 months).
- Net Promoter Score (NPS): This simple survey question (“How likely are you to recommend our practice to a friend or family member?”) is a powerful predictor of patient loyalty and future patient churn.
- Patient Digital Engagement Index (PDEI): A newer metric that measures how actively your patients are using your digital tools, like the patient portal or online scheduling. High PDEI correlates with better engagement.
- No-Show & Cancellation Rates: A high no-show rate is a red flag for poor communication or a difficult scheduling process. A drop in this rate is a clear sign that your engagement strategies, such as those provided by a medical virtual receptionist, are working.
Traditional In-House Staffing vs The VMA Model
When faced with operational overload, the traditional answer is to hire more staff. However, the VMA model offers a more flexible, cost-effective, and scalable solution for the modern practice.
| Feature | Traditional In-House Staff | Care VMA Model |
|---|---|---|
| Cost | High salary, benefits, recruiting, and overhead costs. | Lower-cost subscription model with no overhead. |
| Training | Requires extensive internal training on new tech and workflows. | VMAs are pre-trained on the latest healthcare tech (EHR, RPM, CRM). |
| Flexibility | Fixed hours and roles, difficult to scale up or down. | Fully scalable; add or reduce hours/staff as your needs change. |
| HR Burden | You manage payroll, turnover, and all associated HR tasks. | We handle all HR, ensuring consistent, reliable support. |
FAQ (People Also Ask Optimization)
What are the best patient engagement strategies for 2026?
The best strategies focus on hyper-personalization using patient data, opening a “digital front door” with 24/7 online scheduling, using omnichannel communication (especially two-way SMS), and ensuring proactive continuity of care with automated follow-ups and Remote Patient Monitoring support.
How do you measure patient retention?
Key metrics include the Patient Retention Rate (percentage of returning patients), Net Promoter Score (NPS) to gauge loyalty, and a decrease in No-Show & Cancellation Rates, which indicates an improved scheduling and communication experience.
How can AI improve patient retention?
Artificial Intelligence can analyze EHR data to predict patients at risk of churn, automate personalized outreach at scale, power 24/7 chatbots for instant support, and even assist with documentation through tools like AI Medical Scribes to reduce clinician burnout and improve the in-person experience.
Stop the Churn, Start the Growth
In the new era of Value-Based Care, retaining your patients is the single most powerful financial strategy you can deploy. The challenge is no longer figuring out what to do, but finding who has the time and expertise to do it. Simply adding more software to your tech stack won’t solve the underlying problem of operational overload.
The solution is to integrate a skilled, remote team member who can execute these critical retention tasks for you. A Virtual Medical Assistant from Care VMA is more than just a helping hand—they are a strategic partner dedicated to closing your operational gaps, improving the patient experience, and securing your practice’s financial future.
Ready to see how a VMA can transform your patient retention?


